Begin your 12-day prednisone taper with a carefully planned schedule. We recommend starting at your current dose and reducing it by 5mg every other day. This gradual decrease minimizes withdrawal symptoms and allows your body to adjust naturally.
This schedule provides a structured approach: Days 1-2: current dose; Days 3-4: reduce by 5mg; Days 5-6: new dose; Days 7-8: reduce by another 5mg; Days 9-10: new dose; Days 11-12: final reduction to zero. Always consult your physician to confirm this plan aligns with your specific needs and health conditions.
Note: Closely monitor yourself for potential side effects like fatigue, joint pain, or mood changes. These symptoms are common, but reporting them to your doctor ensures appropriate management. Adequate hydration and a balanced diet support your body throughout the tapering process.
Remember: This is a sample taper; individual needs vary. Your doctor will determine the most appropriate dosage reduction for your unique circumstances. Never alter your medication schedule without consulting a healthcare professional. Regular communication with your doctor throughout this 12-day period is vital for successful completion and to manage any potential issues that arise.
- 12-Day Prednisone Taper: A Detailed Guide
- Sample 12-Day Prednisone Taper Schedule (mg/day)
- Managing Potential Side Effects
- Understanding Prednisone and its Withdrawal Symptoms
- Creating Your Personalized 12-Day Prednisone Taper Schedule
- Monitoring Your Body During the Taper: What to Expect
- Managing Common Side Effects
- When to Contact Your Doctor
- Additional Tips
- Managing Potential Side Effects of Prednisone Withdrawal
- Dietary and Lifestyle Adjustments for a Smooth Taper
- When to Contact Your Doctor: Recognizing Warning Signs
- Other Reasons to Call Your Doctor:
- Maintaining Long-Term Health After Prednisone Treatment
12-Day Prednisone Taper: A Detailed Guide
Always follow your doctor’s prescribed tapering schedule. This 12-day plan is a sample; adjust only with your physician’s approval. Never abruptly stop prednisone.
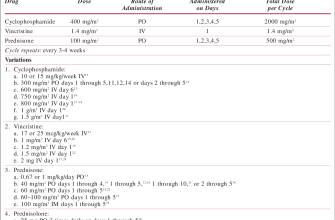
Sample 12-Day Prednisone Taper Schedule (mg/day)
| Day | Prednisone Dose |
|---|---|
| 1-3 | 60 |
| 4-6 | 40 |
| 7-9 | 20 |
| 10-12 | 10 |
This schedule assumes you are currently on 60mg daily. Your doctor will adjust this based on your individual needs and health history. Smaller reductions may be necessary for certain individuals.
Monitor for withdrawal symptoms such as fatigue, joint pain, or muscle weakness. Report any concerning symptoms to your doctor immediately. Staying hydrated is crucial. Maintain a healthy diet, focusing on fruits, vegetables, and lean protein.
Managing Potential Side Effects
Expect some side effects as your body adjusts. These might include increased appetite, insomnia, and mood changes. Regular exercise can help mitigate these. Consider gentle activities like walking or yoga. Get sufficient sleep. Consult your doctor if these side effects are severe or persistent.
This information is for guidance only and does not substitute professional medical advice. Always consult your physician before making changes to your medication regimen.
Understanding Prednisone and its Withdrawal Symptoms
Prednisone is a powerful corticosteroid that suppresses inflammation. While it effectively treats many conditions, abruptly stopping it can cause withdrawal symptoms. A gradual taper, like the 12-day plan, minimizes these effects.
Withdrawal symptoms vary greatly depending on the dosage and duration of prednisone use. Common symptoms include:
- Fatigue
- Muscle weakness
- Joint pain
- Headache
- Nausea
- Loss of appetite
- Dizziness
In more severe cases, you may experience:
- Fever
- Low blood pressure
- Severe joint pain
- Increased anxiety
- Depression
The severity of withdrawal symptoms usually correlates with the prednisone dosage and length of treatment. Higher doses and longer treatment durations increase the risk of more intense withdrawal.
Always follow your doctor’s prescribed tapering schedule. Never stop taking prednisone suddenly. If you experience concerning symptoms during your taper, contact your doctor immediately. They can adjust the schedule or provide additional support.
Managing withdrawal symptoms often involves close monitoring and potential adjustments to the tapering schedule. Your doctor might suggest supplementing with other medications to alleviate specific symptoms.
- Hydration: Drink plenty of water to support your body during the tapering process.
- Diet: Maintain a balanced diet rich in fruits and vegetables.
- Rest: Prioritize rest and avoid strenuous activities.
Remember, a successful prednisone taper requires careful planning and close collaboration with your healthcare provider. Open communication about your symptoms is key to a comfortable withdrawal.
Creating Your Personalized 12-Day Prednisone Taper Schedule
Always consult your doctor before starting any prednisone taper. They will determine the best starting dose and tapering schedule for your specific needs and health condition. A standard 12-day taper isn’t always appropriate.
However, if your doctor approves a 12-day taper, consider these sample schedules. Remember, these are examples; your doctor might prescribe a different plan.
- Option 1: Linear Taper
- Day 1-3: 40mg
- Day 4-6: 30mg
- Day 7-9: 20mg
- Day 10-12: 10mg
- Option 2: Slightly Accelerated Taper
- Day 1-2: 40mg
- Day 3-4: 30mg
- Day 5-7: 20mg
- Day 8-10: 10mg
- Day 11-12: 5mg
Factors influencing your schedule include your initial dose, the reason for prednisone use, and your body’s response to the medication. Your doctor will monitor you closely for any adverse effects. Report any symptoms like fatigue, muscle weakness, or joint pain immediately.
Maintaining a detailed record of your daily dose and any symptoms you experience is crucial. This allows your doctor to make adjustments as needed and ensures your safety during the tapering process. Use a journal or a simple spreadsheet to track this information.
Remember, a gradual reduction is key to minimizing withdrawal symptoms. Do not abruptly stop taking prednisone without consulting your physician. Following your doctor’s instructions carefully is the best way to ensure a safe and successful taper.
Monitoring Your Body During the Taper: What to Expect
Track your weight daily. Sudden changes, especially weight gain, require immediate medical attention. Note any swelling in your ankles or face, too.
Managing Common Side Effects
Expect some fatigue. Rest when needed, but try to maintain a gentle exercise routine. Increased thirst and urination are also possible; ensure adequate hydration. Monitor your blood pressure regularly; some individuals experience temporary increases or decreases.
Pay close attention to your mood. Prednisone can influence emotional well-being; report any significant shifts in mood or anxiety to your doctor. Sleep disturbances are common; prioritize a consistent sleep schedule. You might notice increased appetite; focus on nutritious, balanced meals to avoid excessive weight gain.
When to Contact Your Doctor
Seek immediate medical assistance if you experience severe muscle weakness, chest pain, or difficulty breathing. Contact your doctor if you notice persistent headaches, significant vision changes, or unexplained bruising or bleeding. Also, report any severe or unusual side effects immediately. Your doctor will provide personalized guidance.
Additional Tips
Maintain open communication with your doctor throughout the tapering process. Regular check-ups help ensure your body reacts positively to the reduction. Keep a detailed journal of your symptoms and medications to facilitate clear communication during appointments.
Managing Potential Side Effects of Prednisone Withdrawal
Gradually reduce your prednisone dose as prescribed. This minimizes withdrawal symptoms.
Monitor your blood pressure regularly. Prednisone can elevate blood pressure, and withdrawal can cause sudden drops. Report any significant changes to your doctor.
Consume plenty of potassium-rich foods like bananas, sweet potatoes, and spinach. Prednisone can deplete potassium, increasing the risk of muscle weakness and irregular heartbeat during withdrawal.
Stay hydrated. Drink ample fluids to support your kidneys and overall health during this transition.
Manage fatigue by prioritizing rest. Plan your activities to conserve energy, and don’t hesitate to ask for help.
Expect some joint pain and muscle aches. Light exercise, approved by your doctor, may help manage discomfort; however, avoid overexertion.
Address any mood changes promptly. Prednisone withdrawal can affect mood. Communicate with your doctor about any significant shifts in your emotional state.
Pay attention to your appetite and weight. Your appetite might fluctuate, leading to weight changes. Consult your physician about any concerning variations.
Avoid abrupt cessation. Stopping prednisone suddenly is risky and can trigger severe withdrawal symptoms. Strictly adhere to your doctor’s tapering schedule.
Maintain open communication with your healthcare provider. Regular check-ups help monitor your progress and address any emerging concerns throughout the withdrawal period.
Dietary and Lifestyle Adjustments for a Smooth Taper
Prioritize nutrient-rich foods. Focus on lean proteins like chicken breast, fish, and beans; complex carbohydrates such as brown rice and quinoa; and plenty of fruits and vegetables. This provides sustained energy and supports your body’s natural healing processes.
Stay hydrated. Drink at least eight glasses of water daily. Dehydration can worsen prednisone side effects, so consistent hydration is key.
Manage your blood sugar. Prednisone can elevate blood sugar levels. Choose low-glycemic index foods and limit sugary drinks and processed snacks to avoid sharp spikes.
Monitor your potassium levels. Prednisone can deplete potassium; increase your intake of potassium-rich foods like bananas, sweet potatoes, and spinach. Consult your doctor about supplements if needed.
Reduce stress. Stress exacerbates many prednisone side effects. Incorporate relaxation techniques like yoga, meditation, or deep breathing exercises into your daily routine.
Get adequate sleep. Aim for 7-9 hours of quality sleep each night. Sleep deprivation negatively impacts the body’s ability to recover.
Maintain gentle exercise. Light activity, such as walking, can help manage side effects like fatigue and improve mood. Avoid strenuous exercise, especially during the initial days of the taper.
Listen to your body. Pay attention to how your body responds to the taper and adjust your diet and activity level accordingly. If you experience any concerning symptoms, contact your physician immediately.
Note: This information is for guidance only and does not replace professional medical advice. Always consult your doctor before making significant dietary or lifestyle changes, especially while on prednisone.
When to Contact Your Doctor: Recognizing Warning Signs
Call your doctor immediately if you experience any of the following during your prednisone taper: Severe muscle weakness, significant weight gain (more than 2 pounds in a day), increased thirst and urination, blurred vision, or severe stomach pain. These could signal serious complications.
Other Reasons to Call Your Doctor:
Don’t hesitate to contact your doctor if you notice worsening of your original condition, persistent insomnia despite trying relaxation techniques, unexplained bruising or bleeding, severe mood swings or unusual anxiety, or difficulty breathing. These symptoms, while not always critical, require medical attention to adjust your treatment plan or manage potential side effects.
Remember, open communication with your doctor is key to a successful prednisone taper. Don’t delay seeking help if you have concerns.
Maintaining Long-Term Health After Prednisone Treatment
Schedule regular checkups with your doctor. Monitor your blood pressure and weight closely, reporting any significant changes. This proactive approach helps catch potential issues early.
Gradually increase physical activity. Begin with short walks and progressively increase intensity and duration. Aim for at least 30 minutes of moderate-intensity exercise most days of the week. This supports cardiovascular health and combats potential side effects.
Adopt a balanced diet rich in fruits, vegetables, and lean protein. Reduce processed foods, sugary drinks, and saturated fats. This promotes overall well-being and helps manage weight fluctuations often associated with prednisone.
Prioritize sleep. Aim for 7-9 hours of quality sleep each night. Consistent sleep improves mood, energy levels, and overall health recovery. Consider establishing a relaxing bedtime routine.
Manage stress effectively. Incorporate stress-reducing techniques such as meditation, yoga, or deep breathing exercises. Stress can exacerbate health problems, so proactive management is key.
Maintain open communication with your doctor. Report any new symptoms, concerns, or side effects immediately. Your doctor can provide tailored advice and adjust treatment plans as needed.
Consider bone density testing. Long-term prednisone use can impact bone health. Regular testing helps detect osteoporosis early, allowing for timely intervention.
Pay close attention to your blood glucose levels, especially if you have a history of diabetes or prediabetes. Prednisone can affect blood sugar regulation.
Carefully monitor for signs of infection. Prednisone can suppress the immune system, increasing susceptibility to infections. Seek medical attention promptly if you develop any signs of illness.
Slowly wean yourself off caffeine and alcohol. Both can interfere with sleep and exacerbate some prednisone side effects. Reduce consumption gradually to minimize withdrawal symptoms.