Prednisone significantly impacts your immune system; understand its effects to manage potential risks and maximize benefits. This means paying close attention to dosage and duration, as prolonged use weakens your natural defenses, increasing vulnerability to infections.
Consult your doctor immediately if you experience unusual symptoms like fever, persistent cough, or skin infections while taking prednisone. They can assess your risk and adjust treatment accordingly. Remember, proactive monitoring is key to mitigating potential complications.
Specific actions to take include practicing diligent hand hygiene, avoiding crowded places during flu season, and getting recommended vaccinations. Your physician can provide a personalized plan considering your individual health status and the prednisone regimen.
Proper nutrition and sufficient rest are also paramount to supporting your immune system during prednisone treatment. A balanced diet rich in fruits and vegetables strengthens your body’s natural defenses against infections. Adequate sleep promotes immune cell regeneration, facilitating quicker recovery from any infection.
- Immune System and Prednisone
- How Prednisone Suppresses the Immune System
- Impact on Inflammation and Immune Cell Migration
- Consequences of Prednisone-Induced Immunosuppression
- Common Side Effects of Prednisone Related to Immune Suppression
- Increased Infection Risk: Specifics
- Other Immune-Related Side Effects
- Managing Infection Risk While on Prednisone
- Dietary Considerations
- Recognizing Infection Symptoms
- Medication Adherence
- Seeking Medical Attention
- Preventing Skin Infections
- Prednisone and Long-Term Immune Health
Immune System and Prednisone
Prednisone suppresses your immune system. This means your body’s ability to fight off infections and illnesses decreases. The extent of suppression depends on the dose and duration of treatment.
Higher doses lead to more significant immune suppression. Expect increased susceptibility to infections like colds, flu, and more serious illnesses.
Long-term use poses a greater risk than short-term use. Your doctor will carefully consider the benefits against the risks before prescribing prolonged treatment. Prolonged use increases the likelihood of opportunistic infections – infections caused by microbes usually kept in check by a healthy immune system.
Monitor for infections. Report any signs of infection immediately, such as fever, cough, sore throat, or unusual fatigue. Early treatment is key.
Vaccination is crucial. Discuss vaccination schedules with your doctor, especially for influenza and pneumococcal pneumonia. Your immune response might be weaker while taking prednisone, making vaccinations more critical.
Hygiene is paramount. Frequent handwashing and avoiding contact with sick individuals help minimize infection risk.
Lifestyle choices influence immune function. Maintaining a healthy diet, getting sufficient sleep, and managing stress positively impact your body’s defenses, even while on prednisone.
Regular check-ups are vital. Your doctor will monitor your health and adjust your prednisone dosage as needed, ensuring both disease control and immune system health.
Medications: Always inform your doctor and pharmacist of all medications you take, including over-the-counter drugs and herbal supplements, to avoid potential interactions.
How Prednisone Suppresses the Immune System
Prednisone, a corticosteroid, significantly weakens your immune response. It achieves this primarily by interfering with several key immune cell types and their functions. Specifically, prednisone reduces the production and activity of lymphocytes, including T cells and B cells, crucial for adaptive immunity. This leads to a lower antibody count, making you more susceptible to infections.
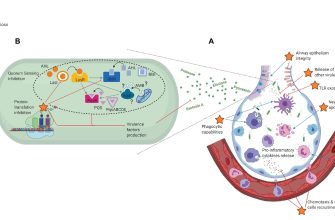
Impact on Inflammation and Immune Cell Migration
Prednisone also dampens the inflammatory response. While inflammation is a vital part of fighting infection, excessive inflammation can harm the body. Prednisone decreases the release of inflammatory cytokines, chemical messengers that orchestrate inflammation. This action also limits the movement of immune cells to sites of infection or injury, further hindering the immune response. This effect can be beneficial in autoimmune diseases but increases infection risk.
Consequences of Prednisone-Induced Immunosuppression
Decreased immune function increases vulnerability to infections, including both common colds and more severe illnesses. The severity of infection risk depends on the prednisone dosage and duration of treatment. Individuals on prednisone should prioritize preventive measures like vaccination and maintaining good hygiene. Always discuss potential side effects and preventative strategies with your physician before starting or adjusting prednisone therapy. They can help manage your risk and develop a plan to address potential problems.
Common Side Effects of Prednisone Related to Immune Suppression
Prednisone weakens your immune system, leaving you more susceptible to infections. Expect a higher risk of common colds, flu, and other illnesses. Monitor your body closely for signs of infection like fever, cough, or sore throat. Report these symptoms to your doctor immediately.
Increased Infection Risk: Specifics
Bacterial, viral, and fungal infections become more likely. This includes opportunistic infections caused by microorganisms normally controlled by a healthy immune system. Pay close attention to any skin changes, such as rashes or sores that don’t heal. Avoid contact with individuals who are ill. Practicing good hygiene, including frequent handwashing, is crucial.
Remember, vaccines might be less effective while on prednisone. Discuss vaccination schedules with your physician. Your doctor might recommend avoiding live vaccines during treatment. Delaying non-urgent procedures that can weaken your immunity is also advisable. Regular check-ups are critical to monitor for any complications.
Other Immune-Related Side Effects
Prednisone can also suppress your body’s natural inflammatory response. While helpful for managing certain conditions, this suppression can delay wound healing. Expect slower recovery from injuries, bruises, and surgeries. Pay extra attention to protecting yourself from injury and ensure proper wound care.
Additionally, you may experience a heightened sensitivity to allergens. This means that allergies you normally manage well might become more severe. Be prepared with appropriate medications and avoid potential triggers. A detailed discussion with your allergist is recommended if allergies worsen significantly.
Managing Infection Risk While on Prednisone
Wash your hands frequently with soap and water for at least 20 seconds, especially before eating and after using the restroom. This simple act significantly reduces your exposure to germs.
Avoid contact with individuals who are sick. Influenza and other common illnesses pose a heightened risk while your immune system is suppressed.
Get recommended vaccinations. Talk to your doctor about the flu shot and pneumococcal vaccine. These vaccines offer crucial protection against serious infections.
Dietary Considerations
Maintain a healthy, balanced diet rich in fruits and vegetables. These foods are packed with nutrients that support immune function.
Stay hydrated by drinking plenty of water throughout the day. Dehydration can weaken your body’s defenses.
Recognizing Infection Symptoms
Pay close attention to any signs of infection, however subtle. These might include fever, cough, sore throat, or unusual fatigue. Report any symptoms to your doctor immediately.
Medication Adherence
Strictly follow your doctor’s instructions regarding prednisone dosage and schedule. Improper use can compromise its effectiveness and increase your vulnerability.
Seeking Medical Attention
Don’t hesitate to contact your doctor if you suspect an infection. Early intervention is key to preventing complications.
| Symptom | Action |
|---|---|
| Fever (100.4°F or higher) | Contact your doctor immediately. |
| Persistent cough | Seek medical advice. |
| Severe sore throat | Schedule an appointment with your physician. |
| Unusual fatigue or weakness | Report this to your doctor. |
Preventing Skin Infections
Keep any cuts or wounds clean and covered with a sterile bandage to prevent infection. Use antiseptic solutions as directed by your physician.
Prednisone and Long-Term Immune Health
Long-term prednisone use significantly impacts your immune system. Understand this impact to mitigate potential risks.
Prednisone suppresses your immune response, leaving you more vulnerable to infections. This effect persists even after you stop taking the drug; the duration depends on the dosage and treatment length.
- Increased Infection Risk: Expect a heightened susceptibility to various infections, including common colds, influenza, and more serious illnesses. Regular handwashing and flu vaccinations are crucial.
- Delayed Wound Healing: Prednisone can hinder your body’s ability to repair tissues. This delays wound healing, making even minor injuries potentially problematic.
- Opportunistic Infections: Your body’s reduced defenses allow opportunistic infections–those caused by microbes usually kept in check by a healthy immune system–to thrive.
Managing these risks requires proactive steps:
- Close Monitoring: Regular check-ups with your doctor are paramount for early detection of potential issues.
- Vaccination: Discuss vaccination schedules with your doctor. You may need extra protection against preventable diseases.
- Hygiene: Practice meticulous hygiene to minimize infection risk.
- Lifestyle Changes: A balanced diet, regular exercise, and sufficient sleep support immune function, even while on prednisone.
- Gradual Tapering: Never abruptly stop prednisone; a gradual reduction under medical supervision minimizes the impact on your immune system.
- Reporting Symptoms: Report any signs of infection promptly to your doctor. Early intervention improves outcomes.
Remember, open communication with your doctor is key. They can tailor advice to your specific needs and medical history, ensuring you receive the best possible care and support throughout and after your prednisone treatment.