No, prednisone is not a narcotic. It’s a corticosteroid, a powerful anti-inflammatory drug. This means it reduces swelling and inflammation in the body, unlike narcotics which primarily affect the central nervous system to relieve pain.
Prednisone works differently. It mimics the effects of cortisol, a hormone naturally produced by your adrenal glands. This hormone regulates various bodily functions, influencing inflammation and immune responses. By increasing cortisol levels, prednisone effectively combats inflammation associated with many conditions, including allergies, asthma, and autoimmune diseases.
While prednisone offers significant therapeutic benefits, it’s crucial to remember it carries potential side effects. These can range from mild, such as increased appetite or trouble sleeping, to more serious ones, like increased blood sugar or weakened bones. Always discuss potential risks and benefits with your doctor before starting or altering your prednisone dosage.
Remember: This information is for educational purposes only and does not substitute professional medical advice. Consult your physician or pharmacist for personalized guidance on prednisone use and management of any potential side effects. They can accurately assess your individual needs and provide the best course of action for your specific health situation.
- Is Prednisone a Narcotic?
- Understanding the Differences
- Prednisone’s Classification: A Corticosteroid, Not a Narcotic
- Key Differences
- Misconceptions
- Understanding Narcotics: Their Defining Characteristics and Effects
- Key Characteristics of Narcotics
- Effects of Narcotic Use
- Prednisone’s Mechanism of Action: How It Differs from Narcotics
- Corticosteroids like Prednisone
- Narcotics (Opioids)
- Key Differences Summarized
- Mechanisms
- Effects
- Common Uses of Prednisone: Inflammatory and Autoimmune Conditions
- Asthma and Allergic Reactions
- Other Inflammatory Conditions
- Potential Side Effects of Prednisone: A Comparison to Narcotic Side Effects
- Prednisone Side Effects
- Narcotic Side Effects
- Comparison Table
- Managing Side Effects
- Prednisone Dependence and Withdrawal: Addressing Concerns
- Seeking Accurate Information: Consulting Medical Professionals for Guidance on Prednisone
Is Prednisone a Narcotic?
No, prednisone is not a narcotic. It’s a corticosteroid, a type of steroid hormone with powerful anti-inflammatory effects. Narcotics, on the other hand, are opioid drugs that relieve pain and can be highly addictive. These medications work through entirely different mechanisms in the body.
Understanding the Differences
Prednisone reduces inflammation by suppressing the immune system. This makes it effective for treating conditions like asthma, allergies, and autoimmune diseases. It does not interact with opioid receptors in the brain, unlike narcotics such as morphine or codeine. While prednisone can have side effects, including mood changes, it doesn’t produce the euphoric effects or physical dependence associated with narcotics.
Always consult your doctor or pharmacist before starting or stopping any medication, including prednisone. They can provide personalized guidance on its appropriate use and help manage potential side effects.
Prednisone’s Classification: A Corticosteroid, Not a Narcotic
Prednisone is a corticosteroid, a type of steroid hormone. It’s not a narcotic. Narcotics, also known as opioids, are a class of drugs that act on the central nervous system to relieve pain and induce drowsiness. They have a high potential for addiction.
Key Differences
Corticosteroids like prednisone reduce inflammation and suppress the immune system. They work differently than narcotics, targeting specific receptors in the body to manage conditions like allergies, asthma, and autoimmune diseases. While prednisone can have side effects, addiction isn’t one of them. However, long-term use should always be monitored by a doctor.
Misconceptions
The confusion might arise because both prednisone and narcotics can be prescribed for pain management, but they operate through vastly different mechanisms. Prednisone addresses inflammation-related pain, while narcotics target pain signals directly in the brain. Always clarify a medication’s classification with your doctor or pharmacist if you have questions.
Understanding Narcotics: Their Defining Characteristics and Effects
Narcotics, also known as opioids, are a class of drugs that act on opioid receptors in the brain and nervous system. This interaction produces significant effects, primarily pain relief, but also including euphoria, sedation, and respiratory depression. Their defining characteristic is their potential for both physical and psychological dependence, leading to addiction with continued use.
Key Characteristics of Narcotics
These drugs share a common mechanism of action, binding to opioid receptors. This binding triggers a cascade of effects throughout the body. Different narcotics have varying potencies and durations of action, affecting how long and intensely their effects are felt. For instance, heroin acts rapidly and intensely, whereas methadone provides a longer-lasting effect, crucial for managing opioid withdrawal. This difference in properties heavily influences treatment strategies.
Effects of Narcotic Use
Pain relief is the primary medical application of narcotics. However, recreational use often focuses on the euphoric effects, a feeling of intense well-being and relaxation. This can lead to tolerance, requiring higher doses to achieve the same effect, raising the risk of overdose. Sedation is another significant effect, potentially leading to slowed breathing and decreased heart rate. Severe respiratory depression is a major cause of narcotic overdose deaths. Withdrawal symptoms, ranging from muscle aches and intense cravings to nausea and vomiting, are a hallmark of narcotic dependence, highlighting the serious nature of addiction.
Prednisone’s Mechanism of Action: How It Differs from Narcotics
Prednisone is a corticosteroid, not a narcotic. This key difference lies in how each drug affects the body.
Corticosteroids like Prednisone
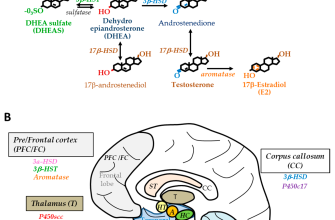
Prednisone works by binding to specific receptors inside cells, influencing gene expression. This impacts various bodily functions, including inflammation reduction, immune system modulation, and metabolism. Think of it as a finely tuned conductor of several biological orchestras.
- Reduces inflammation: Prednisone inhibits the production of inflammatory molecules, leading to decreased swelling and pain.
- Suppresses the immune system: This action is crucial for autoimmune diseases where the immune system attacks the body’s own tissues. However, it also leaves the patient more vulnerable to infections.
- Affects metabolism: Prednisone can alter blood sugar levels and influence fat distribution.
Narcotics (Opioids)
Narcotics, or opioids, act differently. They bind to opioid receptors in the brain and spinal cord, primarily affecting pain perception and potentially causing euphoria and respiratory depression. The effects are much more targeted to the nervous system.
- Pain relief: Opioids reduce pain signals reaching the brain.
- Euphoria: This effect contributes to the potential for addiction.
- Respiratory depression: A serious side effect that can be life-threatening.
Key Differences Summarized
Mechanisms
- Prednisone: Influences gene expression and multiple bodily systems.
- Narcotics: Primarily interact with opioid receptors in the nervous system.
Effects
- Prednisone: Reduces inflammation, suppresses immunity, affects metabolism.
- Narcotics: Reduces pain, can cause euphoria, and suppresses respiration.
In short, prednisone and narcotics work through entirely different mechanisms and produce vastly different effects on the body. Prednisone is an anti-inflammatory and immunosuppressant, while narcotics are potent analgesics with significant risks of addiction and respiratory complications.
Common Uses of Prednisone: Inflammatory and Autoimmune Conditions
Prednisone effectively treats various inflammatory and autoimmune diseases. For example, it frequently manages symptoms of rheumatoid arthritis, reducing joint pain and swelling. Doctors also prescribe it for lupus, a condition causing inflammation throughout the body; prednisone helps control flare-ups.
Asthma and Allergic Reactions
Prednisone provides rapid relief from severe asthma attacks by reducing airway inflammation. It also helps manage severe allergic reactions, reducing symptoms like swelling and breathing difficulties. Remember, it’s a short-term solution for these conditions; long-term use requires discussion with your physician.
Other Inflammatory Conditions
Beyond arthritis and asthma, prednisone finds use in inflammatory bowel disease (IBD), including Crohn’s disease and ulcerative colitis, by calming intestinal inflammation. It also aids in managing certain eye conditions like uveitis and optic neuritis, reducing inflammation and preserving vision. Your doctor will determine the appropriate dosage and duration based on your specific condition and response.
Potential Side Effects of Prednisone: A Comparison to Narcotic Side Effects
Prednisone, a corticosteroid, and narcotics, like opioids, both cause side effects, but they differ significantly. Understanding these differences is vital for managing treatment.
Prednisone Side Effects
Common prednisone side effects include weight gain, increased appetite, mood changes (including irritability and anxiety), insomnia, high blood pressure, and increased risk of infection. Long-term use can lead to more serious problems like osteoporosis, cataracts, and increased blood sugar.
Narcotic Side Effects
Narcotics, conversely, frequently cause drowsiness, constipation, nausea, and respiratory depression. Addiction and tolerance are serious risks with prolonged use. Overdose can be fatal.
Comparison Table
| Side Effect | Prednisone | Narcotics |
|---|---|---|
| Weight Changes | Weight gain common | Weight changes less common, usually loss due to nausea |
| Mood Changes | Irritability, anxiety, mood swings | Euphoria, dysphoria, confusion |
| Gastrointestinal Issues | Increased appetite, rarely serious gastrointestinal upset | Constipation, nausea, vomiting |
| Sleep Disturbances | Insomnia | Drowsiness |
| Respiratory Effects | No direct respiratory depression | Respiratory depression, a serious risk |
| Addiction Potential | Low | High |
Managing Side Effects
Always discuss any side effects with your doctor. They can help manage these using different strategies, such as adjusting dosage or prescribing additional medications.
Prednisone Dependence and Withdrawal: Addressing Concerns
Prednisone isn’t a narcotic, but prolonged use can lead to dependence and uncomfortable withdrawal symptoms. Always follow your doctor’s instructions regarding dosage and tapering. Sudden cessation is strongly discouraged.
Withdrawal symptoms vary greatly depending on the dose and duration of treatment. Commonly reported symptoms include:
- Fatigue
- Muscle weakness
- Joint pain
- Nausea
- Headache
- Low blood pressure
- Fever
In more severe cases, individuals may experience:
- Severe fatigue
- Significant weight loss
- Depression
- Hypotension requiring hospitalization
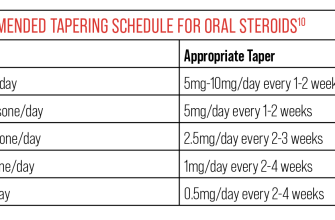
To manage withdrawal, your doctor will likely recommend a gradual tapering schedule. This involves slowly reducing your prednisone dose over several weeks or months. The specific timeframe depends on your individual circumstances, including the dosage and length of your treatment. Never adjust your dosage without consulting your physician.
During the tapering process, monitor your symptoms closely and report any concerns to your doctor. They may be able to adjust your tapering schedule or offer additional support to manage discomfort. Open communication with your healthcare provider is key to successful withdrawal.
Remember, managing prednisone withdrawal effectively requires a collaborative effort between you and your healthcare team. Don’t hesitate to discuss any questions or concerns you have. Your health and well-being are paramount.
Seeking Accurate Information: Consulting Medical Professionals for Guidance on Prednisone
Always discuss prednisone use with your doctor or pharmacist. They can provide personalized advice based on your specific health needs and medical history.
Your doctor will help you understand potential side effects and how to manage them. This includes monitoring for serious side effects and adjusting the dosage as needed.
Pharmacists are another valuable resource. They can answer questions about drug interactions and provide guidance on proper medication usage. Don’t hesitate to contact them with any concerns.
If you experience any unexpected side effects or worsening of your condition while taking prednisone, contact your doctor immediately. Prompt attention to potential complications is critical.
Reliable information about medications comes from your healthcare team and reputable sources like the FDA website and professional medical journals. Avoid relying on unverified online information.
Open communication with your healthcare providers is key to safe and effective prednisone use. Ask questions and express concerns; your health is a priority.