Prednisolone, a corticosteroid, treats inflammation and autoimmune disorders. Always follow your doctor’s instructions; dosage varies greatly depending on the specific condition and individual factors. Never adjust your dosage without consulting your physician.
Common uses include managing asthma, allergic reactions, and inflammatory conditions like arthritis. It’s crucial to understand potential side effects, including weight gain, increased blood sugar, and mood changes. Regular monitoring by your healthcare provider is vital to mitigate these risks. Specific blood tests might be necessary to track your progress and adjust treatment accordingly.
Long-term prednisolone use requires careful management due to the risk of serious side effects. Your doctor will create a tapering schedule to gradually reduce your dosage and minimize withdrawal symptoms. This helps your body adjust naturally, reducing the chance of adverse reactions. Be sure to discuss any concerns you may have with your doctor. Open communication is key to successful treatment.
Remember, this information is for educational purposes only and should not substitute professional medical advice. Consult your physician or pharmacist before starting or changing any medication, including prednisolone. They can assess your individual needs and guide you toward the safest and most effective treatment plan.
- Prednisolone for Humans: A Detailed Guide
- Common Uses
- Possible Side Effects
- Precautions and Interactions
- Withdrawal
- Monitoring
- Alternative Treatments
- Disclaimer:
- What is Prednisolone and How Does it Work?
- How Prednisolone Reduces Inflammation
- How Prednisolone Suppresses the Immune System
- Specific Actions of Prednisolone
- Important Note:
- Types of Prednisolone Administration:
- Common Uses of Prednisolone in Humans
- Dosage and Administration of Prednisolone
- Oral Administration
- Intravenous and Other Routes
- Important Considerations
- Potential Side Effects of Prednisolone
- Interactions with Other Medications
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
- Potassium-Depleting Diuretics
- Antidiabetic Medications
- Warfarin
- Immunosuppressants
- Other Medications
- Prednisolone and Pregnancy/Breastfeeding
- When to Consult a Doctor Regarding Prednisolone
- Monitoring Your Progress
- Adjusting Dosage or Treatment
- Long-Term Use and Withdrawal of Prednisolone
- Managing Withdrawal Symptoms
- Monitoring During Withdrawal
- Alternative Treatments to Prednisolone
- Addressing Specific Conditions
- Lifestyle Changes and Natural Remedies
- Other Medications
- Important Note:
Prednisolone for Humans: A Detailed Guide
Prednisolone treats inflammation and suppresses the immune system. Always follow your doctor’s instructions precisely. Dosage depends entirely on your specific condition and health, so self-medication is dangerous.
Common Uses
- Autoimmune diseases (e.g., lupus, rheumatoid arthritis)
- Allergies (e.g., severe asthma, allergic reactions)
- Inflammation (e.g., from injuries, certain cancers)
- Some eye conditions
- Certain skin conditions
Prednisolone comes in various forms: tablets, liquids, creams, eye drops, and injections. Your doctor chooses the best form for your needs.
Possible Side Effects
Prednisolone can cause side effects, their severity varying based on dosage and duration of use. Common side effects include:
- Weight gain
- Increased appetite
- Mood changes (anxiety, depression)
- High blood sugar
- High blood pressure
- Fluid retention
- Weakened immune system
- Thinning skin
More severe side effects are less common but require immediate medical attention. These include: severe stomach pain, vision problems, and severe infections.
Precautions and Interactions
Before starting prednisolone, inform your doctor about all medications you are currently taking, including over-the-counter drugs and herbal remedies. This is crucial because prednisolone can interact with many other medications.
Withdrawal
Stopping prednisolone abruptly can be harmful. Your doctor will carefully reduce your dosage gradually to minimize withdrawal symptoms, which can mimic the original condition.
Monitoring
Regular check-ups are necessary while you are taking prednisolone. Your doctor will monitor your blood pressure, blood sugar, and overall health.
Alternative Treatments
Your doctor may suggest alternative treatments depending on your condition and response to prednisolone. Discuss this with your healthcare provider thoroughly.
Disclaimer:
This information is for educational purposes only and does not substitute professional medical advice. Always consult a doctor before starting or stopping any medication.
What is Prednisolone and How Does it Work?
Prednisolone is a corticosteroid medication, a synthetic version of a hormone your body naturally produces. It works by reducing inflammation and suppressing your immune system.
How Prednisolone Reduces Inflammation
Prednisolone mimics the effects of cortisol, a natural hormone that regulates inflammation. It binds to specific receptors in your cells, triggering a cascade of events that decrease the production of inflammatory substances. This leads to a reduction in swelling, redness, pain, and other symptoms of inflammation.
How Prednisolone Suppresses the Immune System
- Prednisolone lowers the activity of your immune cells, like lymphocytes and macrophages, which are key players in inflammatory and immune responses.
- This suppression helps reduce the body’s reaction to allergens, autoimmune diseases, and other conditions involving excessive immune activity.
Specific Actions of Prednisolone
- It stabilizes lysosomal membranes, preventing the release of enzymes that contribute to tissue damage.
- It inhibits the production of prostaglandins and leukotrienes, powerful inflammatory mediators.
- It affects the activity of various other cells and molecules involved in the inflammatory process.
Important Note:
Prednisolone is a powerful medication with potential side effects. Always follow your doctor’s instructions carefully. Never stop taking it abruptly without consulting your physician.
Types of Prednisolone Administration:
- Oral tablets
- Liquid suspensions
- Intravenous or intramuscular injections (in certain situations)
Common Uses of Prednisolone in Humans
Prednisolone treats various inflammatory and autoimmune conditions. Doctors frequently prescribe it for allergies, reducing symptoms like swelling and itching. It’s also a key medication in managing asthma, decreasing airway inflammation and improving breathing.
Rheumatoid arthritis and other inflammatory joint diseases often benefit from prednisolone’s anti-inflammatory effects, easing pain and stiffness. Similarly, it helps manage lupus symptoms by reducing inflammation and tissue damage.
Certain eye conditions, such as uveitis, respond well to prednisolone’s ability to reduce inflammation in the eye. It’s also used in treating skin conditions like eczema and psoriasis by suppressing the immune response that causes these inflammatory reactions.
Prednisolone can also be part of treatment plans for certain cancers, reducing swelling and other side effects from chemotherapy. Doctors may also use it in treating severe cases of inflammatory bowel disease, like Crohn’s disease and ulcerative colitis.
Finally, prednisolone finds application in managing severe allergic reactions and certain types of shock, providing crucial relief from inflammation. Always consult a doctor before using prednisolone or altering your treatment plan.
Dosage and Administration of Prednisolone
Prednisolone dosage depends heavily on the specific condition being treated, the patient’s age, weight, and overall health. Always follow your doctor’s prescription precisely. Never adjust the dosage yourself.
Oral Administration
Prednisolone is often administered orally, usually as tablets or liquid. Typical dosages range from 5mg to 60mg daily, but this varies considerably. Your doctor will determine the appropriate starting dose and any necessary adjustments based on your response to treatment. Take prednisolone as directed, usually with food, to minimize stomach upset. Maintaining a consistent schedule is key to maximizing therapeutic benefit.
Intravenous and Other Routes
In certain situations, prednisolone may be given intravenously (IV) or through injection. This route is often used for severe conditions requiring rapid action. Your healthcare provider will carefully monitor your response and adjust the dosage accordingly. Other less common methods include topical applications (creams or ointments) for skin conditions, and eye drops or nasal sprays for specific localized issues.
Important Considerations
Tapering: When discontinuing prednisolone, it’s crucial to gradually reduce the dosage (tapering) as advised by your doctor to prevent withdrawal symptoms. Sudden cessation can lead to serious adverse effects. Monitoring: Regular monitoring by your doctor is necessary to assess your response to treatment and identify any potential side effects. Side effects: Prednisolone can cause various side effects, including weight gain, increased blood sugar, and changes in mood. Report any concerning symptoms to your doctor immediately. Always discuss any potential drug interactions with your doctor or pharmacist before starting prednisolone.
Potential Side Effects of Prednisolone
Prednisolone, while effective, can cause various side effects. Their severity depends on the dosage and duration of treatment. Always discuss potential risks with your doctor.
Common side effects often include increased appetite leading to weight gain, mood swings (including irritability and anxiety), difficulty sleeping (insomnia), and increased sweating.
Less common, but potentially serious, side effects involve increased blood sugar levels (hyperglycemia), potentially worsening existing diabetes; high blood pressure (hypertension); thinning of the bones (osteoporosis), increasing fracture risk; fluid retention causing swelling (edema); and a weakened immune system, making you more susceptible to infections.
Gastrointestinal issues such as heartburn, stomach ulcers, and nausea can also occur. If you experience severe stomach pain, seek immediate medical attention.
Long-term use significantly increases the risk of cataracts and glaucoma. Regular eye exams are advisable during prolonged prednisolone therapy.
Skin changes like thinning skin, easy bruising, and acne are also possible. Protecting your skin from sun exposure is crucial to mitigate these effects.
Mental health impacts can range from mild mood changes to more severe psychological effects like depression and psychosis, especially with high doses. Report any significant mood changes to your physician.
This is not an exhaustive list. Your doctor can provide more tailored information based on your individual health profile and treatment plan. Always inform your doctor about all medications you are taking to avoid harmful drug interactions.
Interactions with Other Medications
Always inform your doctor about all medications you are taking, including over-the-counter drugs, herbal supplements, and vitamins, before starting prednisolone. This includes prescription medications, even if you haven’t used them recently. Prednisolone can interact negatively with several drug classes.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
Combining prednisolone with NSAIDs, such as ibuprofen or naproxen, increases the risk of stomach ulcers and bleeding. Your doctor might recommend alternative pain management strategies.
Potassium-Depleting Diuretics
Prednisolone can lower potassium levels. Concurrently using potassium-depleting diuretics (water pills) intensifies this effect, potentially leading to dangerous heart rhythm problems. Regular potassium level monitoring is necessary.
Antidiabetic Medications
Prednisolone can raise blood sugar levels. This can negatively affect blood glucose control in patients with diabetes who are on insulin or oral hypoglycemics. Dosage adjustments of these medications may be required. Close monitoring of blood sugar is crucial.
Warfarin
Prednisolone can interfere with how well warfarin (a blood thinner) works. This can increase bleeding risk. Regular blood tests are needed to check the warfarin’s effectiveness.
Immunosuppressants
Using prednisolone alongside other immunosuppressants increases the risk of infections and other side effects. Your doctor will carefully monitor your condition.
Other Medications
Several other drug classes may interact with prednisolone, including medications for heart conditions, osteoporosis, and mental health. Always provide a complete medication list to your physician to ensure your safety.
| Medication Class | Potential Interaction | Monitoring Required |
|---|---|---|
| Digoxin | Increased risk of digoxin toxicity | Regular blood tests |
| Oral contraceptives | Reduced effectiveness of oral contraceptives | Consider alternative contraception methods |
| Rifampin | Reduced effectiveness of prednisolone | Dosage adjustments may be necessary |
This information is not exhaustive, and individual reactions can vary. Always consult your healthcare provider for personalized advice on managing potential drug interactions while taking prednisolone.
Prednisolone and Pregnancy/Breastfeeding
Prednisolone use during pregnancy requires careful consideration. While it crosses the placenta, the risk to the fetus depends heavily on dosage and gestational age. High doses and prolonged use in early pregnancy are associated with increased risks of cleft palate and other birth defects. Your doctor will weigh the potential benefits of treatment against these risks. Lower doses in later pregnancy pose a lower risk.
Prednisolone is excreted in breast milk. While the amount is generally small, it’s important to discuss breastfeeding with your doctor. They can help you assess if the benefits of breastfeeding outweigh any potential risks to your baby, potentially suggesting monitoring the infant’s growth and development.
Always inform your healthcare provider about your pregnancy or breastfeeding plans before starting or continuing prednisolone treatment. They will monitor you and your baby closely to minimize potential adverse effects. Individual risk assessment is critical.
This information is for guidance only and does not replace professional medical advice. Always consult your doctor or other qualified healthcare provider for any questions you may have regarding prednisolone and its effects on pregnancy or breastfeeding.
When to Consult a Doctor Regarding Prednisolone
Contact your doctor immediately if you experience any of the following while taking Prednisolone: severe stomach pain, vomiting blood, black or bloody stools, difficulty breathing, rapid weight gain, swelling in your legs or ankles, severe headache, vision changes, or changes in your mood, including increased anxiety or depression. These could be signs of serious side effects.
Monitoring Your Progress
Schedule regular check-ups with your doctor as prescribed. This allows for monitoring of blood pressure, blood sugar, and bone density – factors that Prednisolone can influence. Openly discuss any concerns or new symptoms, even minor ones. Regular monitoring minimizes the risk of complications.
Adjusting Dosage or Treatment
Never adjust your Prednisolone dosage without consulting your doctor. Sudden changes can be harmful. If you experience side effects or your condition worsens, they can help adjust the dosage or explore alternative treatment options. Report any difficulties with medication adherence – missing doses or having trouble with the treatment plan. Your doctor can provide guidance and support.
Long-Term Use and Withdrawal of Prednisolone
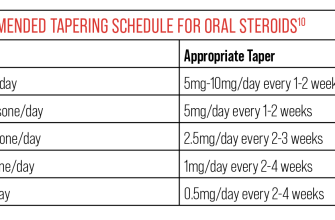
Prednisolone’s prolonged use necessitates a gradual tapering schedule to minimize withdrawal symptoms. Your doctor will create a personalized plan, typically reducing the dose by a small amount every few days or weeks. This slow reduction allows your body to adjust naturally.
Managing Withdrawal Symptoms
Expect potential side effects during withdrawal, including fatigue, muscle weakness, joint pain, and mood changes. These are often temporary and manageable. Your physician might suggest strategies like increased rest, pain management techniques, and potentially short-term use of alternative medications to alleviate these symptoms. Maintaining a healthy diet and regular exercise can also support your body’s recovery.
Monitoring During Withdrawal
Regular check-ups with your doctor are crucial throughout the withdrawal process. They’ll monitor your progress, adjust the tapering schedule as needed, and address any concerning symptoms. Blood tests might be necessary to assess adrenal function, ensuring your body is producing sufficient cortisol.
Alternative Treatments to Prednisolone
Consider the underlying condition requiring Prednisolone. Treating the root cause often minimizes the need for steroids. For example, autoimmune diseases might respond well to biologics like infliximab or adalimumab. These medications target specific components of the immune system, offering a more precise approach than broad-spectrum immunosuppression from Prednisolone.
Addressing Specific Conditions
For allergic reactions, antihistamines like cetirizine or fexofenadine can provide relief. Asthma might benefit from inhaled corticosteroids (like fluticasone) or bronchodilators (like salbutamol). These localized treatments often reduce systemic side effects associated with Prednisolone.
Lifestyle Changes and Natural Remedies
A balanced diet rich in anti-inflammatory foods (like berries and fatty fish) can support the body’s natural healing processes. Regular exercise and stress reduction techniques, such as yoga or meditation, can also significantly impact inflammation levels. Always discuss these options with your doctor before making changes to your treatment plan.
Other Medications
Depending on your specific condition, your doctor might explore other medications. For example, non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can help manage pain and inflammation, but they carry their own risks, so careful monitoring is necessary. Your physician will weigh the benefits and risks to determine the best course of action.
Important Note:
Never stop or change your Prednisolone dosage without consulting your doctor. Switching treatments requires careful monitoring and a gradual transition to prevent complications. Your doctor will help you create a personalized treatment plan based on your individual needs and health status.