Prednisone offers rapid relief during an asthma attack, but understanding its proper use is critical. A short course, typically 5-10 days, often suffices to control inflammation and improve lung function. Remember, exceeding this duration increases the risk of side effects.
Dosage depends on the severity of your exacerbation. Your doctor will determine the appropriate dose based on your symptoms and lung function tests (like peak flow measurements or spirometry). Closely follow their instructions; altering the prescribed dosage without medical advice can be harmful.
Common side effects include weight gain, increased appetite, mood changes, and insomnia. While many are temporary, discuss any concerning side effects immediately with your physician. They can help manage these and adjust treatment as needed. Regular monitoring of blood pressure and blood sugar might also be necessary, especially for individuals with pre-existing conditions.
Remember: Prednisone is a powerful medication; its use should always be guided by a healthcare professional. Self-medicating with prednisone is dangerous and could negatively impact your health. This information provides guidance, but it is not a replacement for personalized medical advice.
- Prednisone’s Role in Asthma Treatment
- Understanding Prednisone’s Mechanism of Action in Asthma
- When is Prednisone Prescribed for Asthma Exacerbation?
- Factors Influencing Prednisone Prescription
- Alternative Treatments and Considerations
- Identifying Triggering Factors and Severity of Exacerbation
- Dosage and Administration of Prednisone for Asthma
- Typical Dosing Regimens
- Administration
- Important Considerations
- Long-Term Use
- Appropriate Dosing Regimens and Potential Side Effects
- Managing Side Effects During Prednisone Treatment for Asthma
- Common Side Effects and Management Strategies
- Less Common, But Important, Side Effects
Prednisone’s Role in Asthma Treatment
Prednisone, a corticosteroid, acts swiftly to reduce airway inflammation, a hallmark of asthma exacerbations. This quick action makes it invaluable for managing severe asthma attacks.
Doctors prescribe prednisone to control symptoms like wheezing, coughing, and shortness of breath. It’s usually a short-term treatment, for days or weeks, not for long-term daily use. Extended use carries significant side effects.
The dosage varies depending on the severity of the asthma exacerbation and the patient’s response. Your doctor will carefully monitor your condition and adjust the dose as needed.
While prednisone offers immediate relief, it doesn’t address the underlying causes of asthma. Therefore, combining prednisone with a long-term asthma control plan is crucial. This plan usually involves inhaled corticosteroids and bronchodilators to prevent future attacks.
| Medication Type | Role in Asthma Management |
|---|---|
| Inhaled Corticosteroids (ICS) | Reduce airway inflammation, preventing exacerbations |
| Bronchodilators | Relax airway muscles, providing quick relief of symptoms |
| Prednisone (Oral Corticosteroid) | Rapidly reduces inflammation during exacerbations |
Common side effects of prednisone include weight gain, increased appetite, mood changes, and sleep disturbances. These usually subside once treatment ends. Discuss any concerns or side effects with your doctor immediately.
Remember, prednisone is a powerful medication, and self-medication is dangerous. Always follow your doctor’s instructions precisely. Regular check-ups and open communication with your healthcare provider are key to managing asthma effectively and safely.
Understanding Prednisone’s Mechanism of Action in Asthma
Prednisone, a glucocorticoid, powerfully reduces airway inflammation in asthma. It achieves this by binding to glucocorticoid receptors inside cells.
This binding initiates a cascade of events. The activated receptor complex then enters the cell’s nucleus, influencing gene expression. Specifically, it reduces the production of inflammatory mediators like leukotrienes and cytokines.
Simultaneously, prednisone increases the production of anti-inflammatory proteins. This helps to counterbalance the inflammatory response, leading to reduced airway swelling, mucus production, and bronchoconstriction.
The result is improved lung function and reduced asthma symptoms. The medication’s effects are typically observed within hours, offering rapid relief during an exacerbation. Remember, consistent use as directed by your physician is key to managing asthma effectively.
When is Prednisone Prescribed for Asthma Exacerbation?
Prednisone, a corticosteroid, treats severe asthma attacks. Your doctor prescribes it when your symptoms don’t respond adequately to your usual inhalers, indicating a moderate or severe exacerbation. Specific triggers include wheezing that doesn’t improve with quick-relief medication, significantly reduced airflow (measured by peak flow meter), increased cough or shortness of breath affecting your daily activities, and worsening nighttime symptoms.
Factors Influencing Prednisone Prescription
Doctors consider several factors: the severity of your symptoms, your response to previous treatments, and your overall health. For instance, a high fever or significantly low oxygen levels will prompt a prednisone prescription more readily. A history of severe asthma exacerbations might lead your physician to prescribe it earlier than for someone with milder, less frequent episodes. Your age and other existing health conditions will also play a role. The duration of treatment and dosage depend on your specific condition and response.
Alternative Treatments and Considerations
While prednisone is effective, it’s important to remember it’s not a long-term solution. Your doctor might explore alternative strategies first, such as increasing the dosage of your usual inhalers. If these methods fail to sufficiently control the exacerbation, prednisone becomes the next treatment option. Always discuss potential side effects and long-term management strategies with your doctor. They will guide you in using prednisone safely and effectively to control your asthma.
Identifying Triggering Factors and Severity of Exacerbation
Accurately identifying the cause of your asthma exacerbation helps your doctor tailor treatment. Keep a detailed diary noting potential triggers and symptoms.
- Common Triggers: Respiratory infections (colds, flu), allergens (pollen, pet dander, dust mites), air pollutants (smoke, smog), irritants (strong odors, perfumes), exercise, stress, and certain medications.
- Symptom Tracking: Note the frequency and severity of wheezing, coughing, shortness of breath, chest tightness, and sputum production. Use a numeric scale (e.g., 0-10) to rate symptom intensity.
Assessing exacerbation severity guides treatment decisions. Consider these factors:
- Peak Expiratory Flow (PEF): Regular PEF monitoring helps detect worsening lung function. Compare your readings to your personal best. Significant drops indicate a more serious exacerbation.
- Oxygen Saturation: Low oxygen levels (below 90%) necessitate immediate medical attention. Use a pulse oximeter for regular monitoring during an exacerbation.
- Respiratory Rate & Effort: Increased respiratory rate (breaths per minute) and visible effort in breathing suggest a severe exacerbation requiring urgent medical care.
- Level of Distress: Note your ability to speak in full sentences, and describe your overall level of discomfort and anxiety. Inability to speak or significant distress requires immediate medical attention.
Based on your recorded data and symptoms, your doctor will determine the appropriate level of care, potentially adjusting Prednisone dosage or adding other treatments.
Remember, prompt action is key. Don’t hesitate to contact your doctor or seek immediate medical attention if your symptoms worsen or you experience any concerning changes in your condition.
Dosage and Administration of Prednisone for Asthma
Prednisone dosage for asthma exacerbations depends on the severity of your symptoms and your individual response to treatment. Your doctor will determine the appropriate dose and duration.
Typical Dosing Regimens
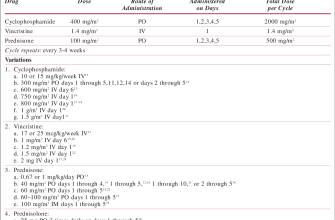
Commonly, a short course of high-dose prednisone (e.g., 40-60 mg daily) is prescribed for several days to quickly control inflammation. The dose is then gradually tapered down over several days or weeks to prevent rebound symptoms and adrenal suppression.
- High-dose initial phase: This usually lasts for 3-10 days, depending on your response. Your doctor will monitor your symptoms carefully.
- Tapering phase: After the initial high-dose phase, your doctor will reduce your daily dosage gradually. This might involve decreasing the dose by 5-10 mg every few days.
The total duration of treatment varies greatly, ranging from a few days to several weeks depending on your individual circumstances.
Administration
Prednisone is typically administered orally, as a tablet or liquid. Always follow your doctor’s instructions carefully regarding how to take the medication.
- Take the medication with food to minimize stomach upset.
- Do not stop taking the medication abruptly without consulting your doctor. Sudden cessation can lead to serious complications.
- Report any side effects to your doctor immediately. Common side effects include increased appetite, weight gain, mood changes, and difficulty sleeping. Serious side effects are less common but require immediate medical attention.
Important Considerations
Long-Term Use
Long-term use of prednisone carries risks, including osteoporosis, cataracts, and increased susceptibility to infections. Your doctor will carefully weigh the benefits and risks before prescribing long-term treatment. In most cases, prednisone is used for short-term management of asthma exacerbations, not for ongoing control.
Disclaimer: This information is for educational purposes only and should not be considered medical advice. Always consult your physician or other qualified healthcare provider before making any decisions related to your health or treatment. They can assess your specific situation and recommend the most appropriate course of action.
Appropriate Dosing Regimens and Potential Side Effects
Prednisone dosages for asthma exacerbations vary depending on severity. A typical starting dose for adults might range from 30-60 mg daily, while children’s doses are significantly lower and always determined by a physician based on weight and severity. This is a short-term treatment, typically lasting only a few days to a week. Gradual tapering is crucial to minimize withdrawal symptoms. Your doctor will create a personalized tapering schedule, usually decreasing the dosage by 5-10 mg every few days.
Potential side effects are a concern. Common ones include increased appetite, weight gain, mood changes, insomnia, and fluid retention. More serious, though less frequent, effects include increased blood sugar, high blood pressure, weakened bones (osteoporosis), and increased risk of infection. Gastrointestinal issues such as heartburn and nausea are also possible.
Regular monitoring is vital. Your physician will likely schedule follow-up appointments to track your progress, adjust medication as needed, and manage potential side effects. Immediate medical attention is necessary if you experience severe side effects like severe abdominal pain, rapid heartbeat, or difficulty breathing.
Open communication with your healthcare provider is key. Report any side effects, no matter how minor they may seem. This allows your doctor to optimize your treatment plan, minimizing risks while ensuring effective asthma control.
Managing Side Effects During Prednisone Treatment for Asthma
Prednisone effectively treats asthma exacerbations, but it can cause side effects. To minimize discomfort, discuss potential side effects with your doctor beforehand. They can help you manage expectations and create a plan.
Common Side Effects and Management Strategies
Increased appetite and weight gain: Focus on nutritious, low-calorie foods. Regular exercise helps counteract calorie intake. Small, frequent meals can aid satiety.
Insomnia: Avoid caffeine and alcohol before bed. Maintain a regular sleep schedule. Consider relaxation techniques like deep breathing or meditation before sleep. If insomnia persists, talk to your doctor; they may adjust your medication schedule or suggest other sleep aids.
Mood changes (irritability, anxiety, depression): Open communication with family and friends is crucial. Regular exercise can improve mood. Your doctor can help assess whether these changes require additional support.
Increased blood sugar: Monitor your blood sugar levels regularly, especially if you have diabetes. Your doctor may recommend adjustments to your diabetes medication. A balanced diet and regular exercise are vital.
Fluid retention: Reduce your sodium intake. Drink plenty of water to flush out excess fluids. Your doctor can monitor for any concerning signs of fluid buildup.
Less Common, But Important, Side Effects
Muscle weakness: Gradually increase physical activity as tolerated, focusing on low-impact exercises. Your doctor can assess the severity and recommend appropriate adjustments.
Increased risk of infection: Practice good hygiene. Avoid crowds during peak flu and cold seasons. Report any signs of infection to your doctor immediately.
Remember, side effects vary. Open communication with your healthcare provider is key to managing them effectively and ensuring safe and successful treatment for your asthma.