Prednisone, a corticosteroid, can significantly reduce inflammation in bronchitis, offering quick relief from symptoms like coughing and shortness of breath. However, it’s not a first-line treatment and carries potential side effects. Your doctor will consider your specific case and overall health before prescribing it.
Expect a reduction in inflammation within a few days of starting Prednisone. This usually translates to less intense coughing and easier breathing. Remember, Prednisone treats symptoms, not the underlying cause of your bronchitis. Therefore, addressing the infection itself remains paramount. This typically involves antibiotics or other appropriate medications, as determined by your doctor.
Potential side effects include increased blood sugar, weight gain, mood swings, and increased risk of infection. Your doctor should carefully monitor you for these during treatment. Never stop taking Prednisone abruptly; tapering off gradually as instructed is crucial to avoid complications. Open communication with your healthcare provider is key to managing this medication safely and effectively.
Long-term Prednisone use for bronchitis is generally not recommended due to the risk of side effects. Your doctor will work with you to find the shortest course of treatment necessary for symptom relief while minimizing potential adverse reactions. A thorough discussion of risks and benefits before starting treatment ensures you are fully informed and can make a well-informed decision.
- Prednisone for Bronchitis: A Detailed Guide
- Understanding Prednisone’s Role
- When Your Doctor Might Prescribe Prednisone
- Potential Side Effects
- Duration of Treatment & Weaning
- Alternative and Complementary Treatments
- Important Note
- What is Prednisone and How Does it Work?
- How Prednisone Treats Bronchitis
- Important Considerations
- Bronchitis: Types and Symptoms
- When is Prednisone Prescribed for Bronchitis?
- Dosage and Administration of Prednisone for Bronchitis
- Potential Side Effects of Prednisone Treatment
- Prednisone and Other Bronchitis Treatments: Combining Therapies
- Long-Term Use of Prednisone and Bronchitis Management
- When to Consult a Doctor Regarding Prednisone and Bronchitis
- Signs Requiring Immediate Medical Attention:
- Reasons to Schedule a Doctor’s Appointment:
- When to adjust Prednisone Dosage:
Prednisone for Bronchitis: A Detailed Guide
Prednisone isn’t a first-line treatment for bronchitis, but your doctor might prescribe it for severe cases or if other treatments fail to provide relief. It works by reducing inflammation in your airways, helping you breathe easier.
Understanding Prednisone’s Role
Prednisone is a corticosteroid that powerfully reduces inflammation. For bronchitis, this means less swelling in your bronchial tubes, leading to improved airflow. This is particularly helpful in acute bronchitis with significant inflammation and wheezing.
When Your Doctor Might Prescribe Prednisone
Your doctor may consider Prednisone if you have severe bronchitis symptoms, such as persistent wheezing, significant shortness of breath, or a high fever unresponsive to other treatments. It can also be useful for those with chronic bronchitis experiencing acute exacerbations. Always follow your doctor’s instructions regarding dosage and duration.
Potential Side Effects
While Prednisone can be highly beneficial, it’s important to be aware of potential side effects, which can include increased blood sugar, weight gain, mood changes, and insomnia. Your doctor will carefully monitor you for these and adjust your treatment as needed. Inform them of any side effects you experience.
Duration of Treatment & Weaning
Prednisone treatment for bronchitis is usually short-term. Your doctor will determine the appropriate dosage and length of treatment based on your individual needs. It’s crucial to follow their instructions closely, including a gradual tapering of the dose to minimize withdrawal effects. Never stop taking Prednisone suddenly without consulting your physician.
Alternative and Complementary Treatments
Alongside Prednisone, your doctor might recommend other treatments such as bronchodilators (to open airways), cough suppressants, or expectorants (to loosen mucus). Lifestyle changes, including adequate hydration and rest, are also crucial for recovery.
Important Note
This information is for educational purposes only and does not constitute medical advice. Always consult your doctor before starting any new medication, including Prednisone. They can assess your specific condition and determine the most appropriate treatment plan for you.
What is Prednisone and How Does it Work?
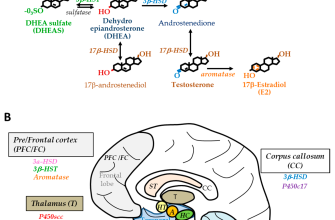
Prednisone is a corticosteroid medication, a powerful anti-inflammatory drug. It mimics the effects of cortisol, a hormone naturally produced by your adrenal glands. This hormone reduces swelling and inflammation throughout your body.
How Prednisone Treats Bronchitis
In bronchitis, your airways become inflamed and irritated. Prednisone targets this inflammation, reducing swelling and allowing for easier breathing. It achieves this by blocking the release of certain chemicals that cause inflammation, and also by suppressing the immune system’s response. This leads to a decrease in mucus production and opens up your airways.
Important Considerations
While Prednisone offers quick relief, it’s crucial to remember it’s not a long-term solution. Long-term use can have side effects, including weight gain, increased blood sugar, and weakened bones. Your doctor will carefully monitor your treatment and prescribe the lowest effective dose for the shortest possible time. Always follow their instructions precisely. Additionally, Prednisone doesn’t address the underlying cause of bronchitis; it only manages symptoms. Your doctor may prescribe other treatments to address the root cause of your illness.
Bronchitis: Types and Symptoms
Bronchitis is broadly categorized into acute and chronic forms. Acute bronchitis, often triggered by viral infections like the common cold or flu, usually resolves within a couple of weeks. Symptoms include a persistent cough, sometimes producing phlegm (mucus), chest discomfort, and shortness of breath. Fever and body aches are also common.
Chronic bronchitis, a more serious condition, involves long-term inflammation of the bronchial tubes. It’s primarily associated with smoking and other respiratory irritants. A persistent cough producing excessive phlegm, especially in the morning, is a hallmark symptom. This cough can last for months, even years. Wheezing and shortness of breath are also frequent.
Differentiating between the two is crucial for proper treatment. While acute bronchitis typically resolves on its own with rest and supportive care, chronic bronchitis requires ongoing management, often involving medications and lifestyle changes to control symptoms and prevent further complications.
Identifying your bronchitis type is a critical first step. Consult a physician for accurate diagnosis and personalized treatment. Early detection and appropriate management significantly impact long-term respiratory health.
Remember, this information is for educational purposes only and does not constitute medical advice. Always seek professional medical guidance for any health concerns.
When is Prednisone Prescribed for Bronchitis?
Prednisone, a corticosteroid, isn’t a first-line treatment for bronchitis. Doctors typically prescribe it for severe cases. This usually means you have acute bronchitis accompanied by significant wheezing, shortness of breath, or a persistent, unproductive cough resistant to other treatments.
Specifically, prednisone might be considered if you have acute exacerbations of chronic obstructive pulmonary disease (COPD) that manifest as bronchitis. Its use in these situations aims to rapidly reduce inflammation and improve breathing.
Another scenario where prednisone may be helpful is when bronchitis is caused by a severe infection, such as whooping cough or a particularly aggressive bacterial infection, and other treatments haven’t provided sufficient relief.
Your doctor will carefully weigh the benefits against the potential side effects before prescribing prednisone. Factors like your overall health and the severity of your bronchitis will heavily influence this decision. Always discuss your treatment options fully with your physician.
Remember, self-treating bronchitis with prednisone is dangerous. Seek professional medical advice before taking any medication, especially corticosteroids.
Dosage and Administration of Prednisone for Bronchitis
Prednisone dosage for bronchitis varies greatly depending on the severity of your condition, your overall health, and your doctor’s judgment. Always follow your doctor’s prescribed dosage and never adjust it without their explicit approval.
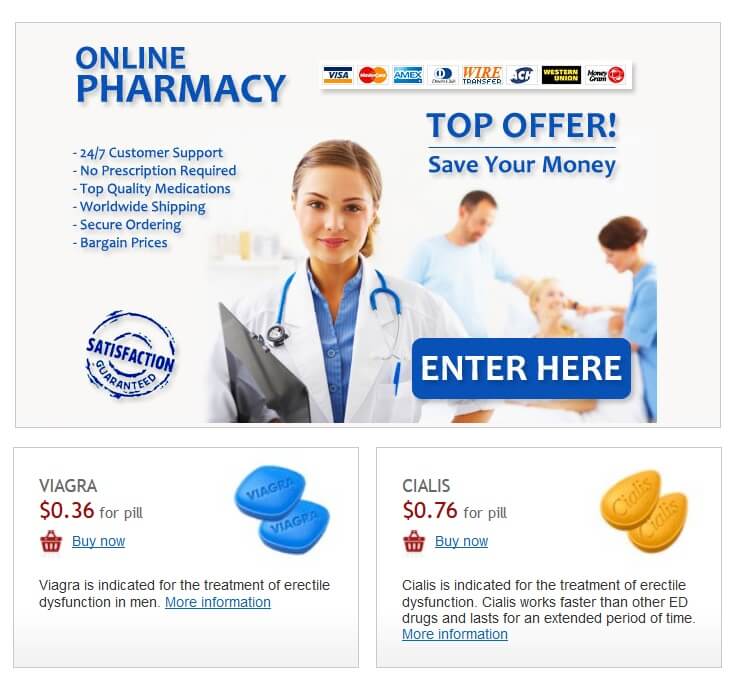
Typically, a short course of prednisone is used for acute bronchitis. This might involve a higher initial dose, gradually decreasing over several days. For example, a common regimen is:
- 40mg daily for the first few days.
- Gradual tapering down by 5-10mg every few days.
- Complete cessation of medication within 7-10 days, depending on your response to treatment.
However, other regimens exist. Your doctor will tailor the treatment to your specific needs.
- Oral Administration: Prednisone is usually taken orally, typically with a meal or snack to minimize stomach upset.
- Timing: Your doctor will specify the best time to take your medication. Consistency is key to successful treatment.
- Missed Dose: If you miss a dose, take it as soon as you remember, unless it’s almost time for your next dose. Don’t double up on doses.
- Side Effects: Be aware of potential side effects like increased appetite, weight gain, mood changes, and sleep disturbances. Report any concerning side effects to your doctor immediately.
Remember, this information is for general knowledge and shouldn’t replace professional medical advice. Always consult your doctor or other qualified healthcare provider for diagnosis and treatment of bronchitis or any medical condition. They will assess your individual needs and determine the appropriate prednisone dosage and administration plan for you.
Potential Side Effects of Prednisone Treatment
Prednisone, while effective in treating bronchitis, can cause various side effects. Understanding these potential issues helps you manage treatment effectively.
Some common side effects include increased appetite leading to weight gain, fluid retention causing swelling (edema), and mood changes, such as irritability or anxiety. You might also experience insomnia or difficulty sleeping.
More serious, though less frequent, side effects require immediate medical attention. These include increased blood sugar levels (hyperglycemia), potentially dangerous for diabetics, and increased risk of infections due to immunosuppression.
Gastrointestinal issues are also possible. Prednisone can cause heartburn, nausea, or ulcers.
Long-term use increases the likelihood of more severe side effects, such as osteoporosis (weakening of bones), cataracts, or glaucoma.
| Side Effect Category | Specific Examples | Action |
|---|---|---|
| Common | Weight gain, edema, mood swings, insomnia | Monitor symptoms; discuss with your doctor if bothersome. |
| Serious | High blood sugar, increased infections, ulcers | Seek immediate medical advice. |
| Long-Term | Osteoporosis, cataracts, glaucoma | Discuss preventative measures with your doctor. |
Always inform your doctor about any new or worsening symptoms. Open communication is key to safe and effective prednisone treatment. Regular monitoring can help minimize risks.
Prednisone and Other Bronchitis Treatments: Combining Therapies
Prednisone often works best alongside other bronchitis treatments. For example, a doctor might prescribe bronchodilators like albuterol to relax airway muscles and improve breathing, complementing Prednisone’s anti-inflammatory action. This combination tackles both the inflammation and the airway constriction contributing to bronchitis symptoms.
Another common pairing involves Prednisone and antibiotics. If your bronchitis is bacterial, antibiotics directly target the infection. Prednisone, simultaneously, manages the inflammation, leading to faster symptom relief and a potentially shorter recovery period. Remember, a doctor must diagnose the bacterial infection before prescribing antibiotics.
Cough suppressants can also be useful alongside Prednisone, particularly if a persistent cough is disrupting sleep or causing discomfort. These medications alleviate the cough without directly addressing the underlying inflammation or infection; Prednisone handles that. This approach provides targeted relief from multiple symptoms.
Hydration remains crucial. Drinking plenty of fluids thins mucus, making it easier to cough up, and aids Prednisone’s action by promoting general wellness. Adequate rest also plays a significant role in facilitating healing during Prednisone treatment and overall bronchitis recovery. Combining these strategies provides a holistic approach.
Your doctor will tailor the combination of treatments to your specific needs, considering your medical history and the severity of your bronchitis. Always discuss potential drug interactions and side effects with your healthcare provider before starting any new medication regime, especially while using Prednisone.
Long-Term Use of Prednisone and Bronchitis Management
Long-term prednisone use for bronchitis requires careful monitoring. Your doctor will likely adjust your dosage gradually to minimize side effects. Expect regular blood tests to check for potential complications, such as high blood sugar or bone thinning.
Lifestyle changes are key. A healthy diet, regular exercise, and stress reduction techniques can significantly improve your condition and reduce reliance on prednisone. Prioritize sleep and avoid irritants like smoke and dust.
Inhalers, such as bronchodilators and corticosteroids, often work alongside prednisone to control inflammation and improve breathing. Your physician will guide you on the appropriate usage and combination of medications.
Regular check-ups are vital. These appointments allow your doctor to assess your progress, adjust your medication plan if needed, and address any emerging health concerns. Open communication is crucial for effective management.
Consider pulmonary rehabilitation programs. These programs offer tailored exercise plans and education to enhance respiratory function and overall well-being. They can help manage bronchitis symptoms even while tapering off prednisone.
Weaning off prednisone should always be gradual, as sudden cessation can trigger a relapse or withdrawal symptoms. Your doctor will create a personalized tapering schedule based on your individual response to treatment. Closely follow their instructions.
When to Consult a Doctor Regarding Prednisone and Bronchitis
Seek immediate medical attention if you experience difficulty breathing, chest pain, or a worsening cough while taking Prednisone for bronchitis. These could indicate serious complications.
Signs Requiring Immediate Medical Attention:
- Severe shortness of breath or wheezing.
- Chest pain or pressure.
- High fever (above 101°F or 38.3°C).
- Cough producing green or yellow mucus.
- Increased confusion or disorientation.
- Rapid heart rate.
Schedule a doctor’s appointment if your bronchitis symptoms don’t improve after several days of Prednisone treatment, or if they worsen. This includes persistent cough, fatigue, and continued production of mucus.
Reasons to Schedule a Doctor’s Appointment:
- Bronchitis symptoms persist for more than 7-10 days despite Prednisone treatment.
- You experience new or worsening symptoms like muscle aches, headaches, or skin rashes.
- You have concerns about side effects of Prednisone, such as increased blood sugar, mood changes, or insomnia.
- You have questions about your Prednisone dosage or treatment plan.
Remember, timely medical intervention can prevent serious health problems. Don’t hesitate to contact your healthcare provider if you have any concerns.
When to adjust Prednisone Dosage:
Never adjust your Prednisone dosage without consulting your doctor. Doing so can have serious health consequences. Always follow your physician’s instructions carefully.