Finding the right Prednisone dosage for asthma control is crucial. Your doctor will personalize your treatment based on your specific needs, considering factors like your age, asthma severity, and response to other medications. Typical starting doses range from 20-60mg daily for adults, often administered as a single dose or divided throughout the day.
The treatment duration depends entirely on the severity of your asthma symptoms. Short courses, lasting a few days to a week, are often used for acute exacerbations. Longer courses might be necessary for severe or persistent asthma, but these should be carefully managed by your physician to minimize side effects. Remember, Prednisone is usually not a long-term solution for managing asthma.
Important Considerations: Close monitoring of your condition is necessary. Your doctor will likely adjust your dosage based on your response. Common side effects include increased appetite, weight gain, mood changes, and sleep disturbances. Report any adverse effects immediately to your doctor. They can help mitigate these side effects or adjust your treatment plan accordingly. Always follow your doctor’s instructions precisely for optimal results and minimizing potential risks.
Note: This information is for general knowledge and does not substitute professional medical advice. Consult your physician for accurate diagnosis and personalized treatment.
- Prednisone Dose for Asthma: A Detailed Guide
- Short-Term Treatment of Asthma Exacerbations
- Tapering the Dose
- Long-Term Prednisone Use for Asthma
- Side Effects
- Alternative and Adjunctive Therapies
- Disclaimer:
- Understanding Prednisone’s Role in Asthma Treatment
- Short-Term vs. Long-Term Use
- Managing Side Effects
- Determining the Appropriate Prednisone Dosage for Asthma Severity
- Dosage Adjustments and Monitoring
- Tapering Prednisone
- Short-Term Prednisone Use for Asthma Exacerbations
- Dosage Adjustments
- Potential Side Effects and Management
- Monitoring Progress
- Example Prednisone Tapering Schedule (Adult):
- Long-Term Use Considerations
- Long-Term Prednisone Use for Asthma: Risks and Benefits
- Prednisone Dosage Adjustments Based on Patient Factors (Age, Weight, etc.)
- Common Side Effects of Prednisone and How to Manage Them
- Tapering Off Prednisone: A Gradual Approach to Minimize Withdrawal Symptoms
- Alternative Treatments and When to Consider Them
- Biologics
- Leukotriene Modifiers
- Lifestyle Changes
- Alternative Therapies and Considerations
- Treatment Selection: A Summary Table
- When to Seek Immediate Medical Attention Regarding Prednisone and Asthma
Prednisone Dose for Asthma: A Detailed Guide
Prednisone dosages for asthma vary greatly depending on the severity of your symptoms and your individual response to treatment. Your doctor will determine the appropriate dose for you. Generally, treatment involves short courses of high-dose prednisone for acute exacerbations, followed by a gradual tapering of the dose.
Short-Term Treatment of Asthma Exacerbations
For severe asthma attacks requiring immediate relief, your doctor might prescribe a high dose, such as 40-60 mg daily for a few days. This high dose helps quickly reduce inflammation and improve breathing. The exact dosage and duration will depend on your specific needs.
- Important Note: Never adjust your prednisone dose without consulting your doctor. Sudden changes can be harmful.
Tapering the Dose
Once your symptoms improve, your doctor will gradually reduce your prednisone dosage. This process, called tapering, helps prevent withdrawal symptoms and minimizes side effects. A typical tapering schedule might involve reducing the dose by 5-10 mg every few days, or according to your doctor’s specific instructions.
- Day 1-3: High dose (e.g., 60mg)
- Day 4-6: Reduced dose (e.g., 50mg)
- Day 7-9: Further reduced dose (e.g., 40mg)
- …and so on, until the dose is completely stopped.
Your doctor will monitor your progress closely during the tapering period. This ensures the gradual reduction is safe and effective for you.
Long-Term Prednisone Use for Asthma
Long-term use of prednisone for asthma is generally avoided due to potential side effects. It’s usually only considered for severe, persistent asthma that doesn’t respond to other treatments. If long-term use is necessary, your doctor will meticulously manage your dose and carefully monitor your health.
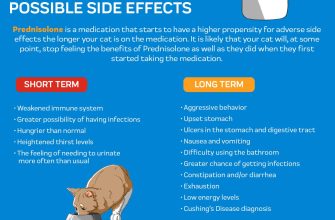
Side Effects
Prednisone can have several side effects, including weight gain, increased appetite, mood changes, insomnia, and increased risk of infections. Open communication with your doctor about any side effects you experience is crucial. They can help manage these effects and adjust your treatment plan accordingly.
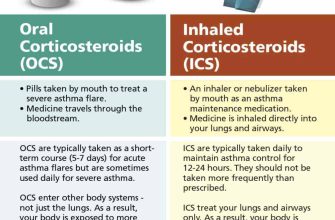
Alternative and Adjunctive Therapies
Prednisone is often used in conjunction with other asthma treatments, such as inhaled corticosteroids and bronchodilators. These medications work synergistically to control inflammation and improve lung function. Your doctor will create a personalized treatment plan that combines the most appropriate medications for your individual needs.
Disclaimer:
This information is for educational purposes only and does not constitute medical advice. Always consult with your doctor or other qualified healthcare professional for diagnosis and treatment of any medical condition.
Understanding Prednisone’s Role in Asthma Treatment
Prednisone, a corticosteroid, acts quickly to reduce airway inflammation, a hallmark of asthma attacks. This rapid anti-inflammatory effect makes it a crucial medication for managing severe asthma exacerbations. Doctors prescribe it to lessen symptoms like wheezing, coughing, and shortness of breath. The dosage and duration depend entirely on the severity of your asthma and your response to treatment. Always follow your doctor’s instructions precisely.
Short-Term vs. Long-Term Use
Prednisone is typically used for short-term management of severe asthma attacks or flare-ups. Long-term daily use carries significant risks, including osteoporosis, cataracts, and increased blood sugar. Your doctor will consider these risks carefully before prescribing long-term prednisone therapy. They might explore alternative long-term asthma control medications like inhaled corticosteroids, long-acting beta-agonists, or biologics instead.
Managing Side Effects
Prednisone can cause several side effects, including weight gain, increased appetite, mood changes, and sleep disturbances. These are often dose-dependent and generally resolve once treatment stops. If you experience any concerning side effects, contact your healthcare provider. They can discuss strategies to minimize these, such as careful diet management or other supportive therapies.
Determining the Appropriate Prednisone Dosage for Asthma Severity
Prednisone dosage for asthma depends entirely on the severity of your symptoms and the patient’s individual response. Your doctor will determine the correct dose, but generally, treatment begins with a short course of high-dose prednisone for acute exacerbations. Typical starting doses range from 30-60mg daily for adults, adjusted based on factors like age, weight, and response. Children receive a significantly lower dose, calculated based on their weight and severity of symptoms. Always follow your doctor’s prescribed regimen.
Dosage Adjustments and Monitoring
Doctors frequently adjust the dosage based on your response. If symptoms improve quickly, the dose might be gradually reduced over several days to minimize side effects. However, if symptoms persist or worsen, the dose may need to increase. Regular monitoring of lung function, using peak flow meters or spirometry, is critical in guiding dose adjustments. Blood tests may also be utilized to assess inflammatory markers. The goal is to find the lowest effective dose that manages your symptoms while minimizing side effects like weight gain, mood changes, or increased blood sugar. Long-term use often requires careful monitoring to mitigate long-term risks.
Tapering Prednisone
Sudden cessation of prednisone after prolonged use can lead to a relapse of asthma symptoms or adrenal insufficiency. Therefore, your doctor will likely gradually reduce (taper) your dose over time. The tapering schedule is individualized and depends on the duration of treatment and your response. Close collaboration with your physician throughout the tapering process is critical to prevent complications and ensure safe discontinuation.
Short-Term Prednisone Use for Asthma Exacerbations
Short bursts of prednisone effectively reduce inflammation during asthma attacks. Doctors typically prescribe a course lasting 5-10 days, depending on the severity of the exacerbation. The most common dosage for adults is 40-60mg daily, often tapered down over several days to minimize side effects. Children receive lower doses, adjusted for their weight and age.
Dosage Adjustments
Your doctor will adjust the prednisone dose based on your specific needs and response to treatment. Factors considered include the severity of your symptoms (wheezing, cough, shortness of breath), lung function tests (peak flow or spirometry), and your overall health. Always follow your doctor’s instructions precisely.
Potential Side Effects and Management
While prednisone is helpful, it can cause side effects. These can include increased appetite, weight gain, mood changes, insomnia, and increased blood sugar. These effects are usually temporary and resolve once you stop taking the medication. Proper hydration and a balanced diet can help mitigate some of these side effects. Inform your doctor about any concerning side effects.
Monitoring Progress
Regular monitoring is crucial. You’ll likely need to track your symptoms and possibly undergo further lung function tests to assess the treatment’s effectiveness. This allows your doctor to make adjustments to the treatment plan if necessary.
Example Prednisone Tapering Schedule (Adult):
| Day | Dose (mg) |
|---|---|
| 1-5 | 60 |
| 6-8 | 40 |
| 9-10 | 20 |
Note: This is a sample schedule. Your doctor will determine the appropriate tapering schedule for you.
Long-Term Use Considerations
Prednisone is not intended for long-term asthma management. Consistent use of your daily controller medications (inhalers) is essential for preventing exacerbations. Discuss long-term asthma control strategies with your doctor.
Long-Term Prednisone Use for Asthma: Risks and Benefits
Prednisone, while highly effective for controlling severe asthma exacerbations, carries significant risks with prolonged use. Doctors rarely prescribe it for long-term asthma management due to these potential drawbacks.
Benefits: Short-term prednisone significantly reduces airway inflammation and improves breathing. This rapid effect makes it invaluable during severe asthma attacks.
- Quick symptom relief.
- Improved lung function.
Risks: Long-term prednisone use presents considerable health challenges.
- Osteoporosis: Prednisone weakens bones, increasing fracture risk. Regular bone density monitoring is crucial.
- Increased Blood Sugar: It can elevate blood sugar levels, potentially leading to diabetes or worsening existing diabetes.
- Weight Gain: Fluid retention and changes in metabolism often cause weight gain.
- High Blood Pressure: Prednisone can raise blood pressure, necessitating monitoring and potential medication adjustments.
- Cataracts and Glaucoma: Long-term use increases the risk of eye problems.
- Weakened Immune System: It suppresses the immune system, making you more susceptible to infections.
- Mood Changes: Prednisone can affect mood, leading to anxiety, irritability, or depression.
- Muscle Weakness: It can cause muscle wasting and weakness.
- Growth Suppression (in children): Prednisone can stunt growth in children.
Alternatives: Long-term asthma management focuses on preventative strategies. Inhaled corticosteroids, long-acting beta-agonists, and other controller medications are preferred for daily use. These medications minimize the need for high-dose steroids.
- Discuss your asthma management plan thoroughly with your doctor.
- Adhere strictly to your prescribed medication regimen.
- Monitor your health closely for any side effects.
- Regularly check your lung function.
Always consult your doctor before making any changes to your medication. They can help determine the best course of action for managing your asthma.
Prednisone Dosage Adjustments Based on Patient Factors (Age, Weight, etc.)
Prednisone dosages for asthma are highly individualized. Doctors carefully consider several factors to determine the appropriate dose. Let’s examine these key elements:
- Age: Children generally require lower doses per kilogram of body weight than adults. Infants and toddlers need particularly careful monitoring due to their developing systems. Always follow a physician’s precise instructions.
- Weight: Dosage is often calculated based on body weight (mg/kg). Heavier individuals may need higher doses, but this isn’t always a linear relationship. Other factors influence the final prescription.
- Asthma Severity: Mild asthma attacks require a far lower dose than severe exacerbations requiring hospitalization. The doctor determines the severity based on the patient’s symptoms and lung function tests.
- Response to Treatment: If the initial dose doesn’t provide sufficient relief, the doctor may increase it. Conversely, if side effects are prominent, a dose reduction might be necessary. Regular monitoring and feedback are crucial.
- Other Medical Conditions: Existing health issues, like liver or kidney disease, can affect how the body processes prednisone, necessitating dose adjustments. The physician considers all pre-existing conditions.
- Medication Interactions: Some medications interact with prednisone, potentially increasing or decreasing its effectiveness. This must be carefully considered, requiring potentially altered dosages.
Remember: This information is for general understanding. Never adjust your prednisone dosage without consulting your doctor. Self-adjusting could lead to serious complications. Always follow your physician’s specific instructions for medication management.
- Seek Medical Advice: This information doesn’t replace professional medical guidance. Contact your physician or other healthcare provider immediately for concerns regarding asthma management or prednisone use.
- Accurate Reporting: Always accurately report all medications, supplements, and allergies to your doctor to ensure appropriate and safe prednisone administration.
Common Side Effects of Prednisone and How to Manage Them
Prednisone, while effective for asthma, can cause side effects. Managing these is key to successful treatment. Common side effects include weight gain, mainly due to fluid retention and increased appetite. Reduce this by following a balanced diet low in processed foods and sodium, and increase your physical activity.
Increased appetite often accompanies this. Focus on nutritious choices and portion control. Regular exercise also helps manage appetite.
Mood swings are another potential side effect. Increased irritability and anxiety can occur. Regular exercise and stress-reduction techniques, like meditation or deep breathing, can help. Communicate openly with your doctor if you experience significant mood changes.
Insomnia is also a possibility. Establish a regular sleep schedule; maintain a relaxing bedtime routine; avoid caffeine and alcohol before bed. Your doctor may suggest alternative sleep aids if necessary.
Prednisone can increase blood sugar. Monitor your blood sugar levels regularly, especially if you have diabetes. Discuss your sugar control plan with your physician; they may adjust your diabetes medication.
High blood pressure is another potential risk. Follow a low-sodium diet, engage in regular physical activity, and monitor your blood pressure regularly. Your doctor can provide guidance and medication if needed.
Remember: These are common side effects; not everyone experiences them. Always discuss any concerns with your doctor. They can help you manage side effects and adjust your treatment plan accordingly. This information does not substitute medical advice. Consult your doctor or pharmacist for personalized guidance.
Tapering Off Prednisone: A Gradual Approach to Minimize Withdrawal Symptoms
Never stop Prednisone abruptly. Your doctor will create a personalized tapering schedule, usually reducing your dose by a small amount every few days or weeks. This gradual decrease allows your body to adjust, minimizing potential side effects.
Common withdrawal symptoms include fatigue, muscle weakness, joint pain, and headaches. These symptoms are usually manageable and temporary. Staying hydrated and eating a balanced diet helps.
Closely monitor your asthma symptoms during the tapering process. If your asthma worsens, contact your doctor immediately. They may adjust your tapering schedule or prescribe additional medication.
Some people experience more severe withdrawal symptoms. Your doctor can prescribe additional medication to manage these, such as low-dose prednisone or other drugs to alleviate specific symptoms.
Regular communication with your doctor is key. Report any concerns or changes in your condition throughout the tapering period. Your doctor will provide the best advice for your individual needs and monitor your progress.
Following your doctor’s instructions precisely is crucial for a safe and successful tapering process. This ensures you manage your asthma effectively while minimizing the discomfort of withdrawal.
Alternative Treatments and When to Consider Them
For many, inhaled corticosteroids remain the cornerstone of asthma management. However, some individuals may require additional therapies or explore alternatives. Let’s explore some options.
Biologics
Biologics target specific parts of the immune system involved in asthma inflammation. They are typically reserved for patients with severe asthma not adequately controlled with other medications. Examples include omalizumab, mepolizumab, and dupilumab. Discuss these with your doctor to determine if they’re suitable for your needs. Specific eligibility criteria exist based on your asthma severity and other factors.
Leukotriene Modifiers
Leukotriene modifiers, like montelukast and zafirlukast, block leukotrienes, chemicals contributing to airway inflammation. These medications can be useful as add-on therapy to improve asthma control, especially in patients with allergies or exercise-induced bronchospasm. They’re not a first-line treatment but a valuable addition when needed.
Lifestyle Changes
Adopting healthy habits can significantly impact asthma control. Regular exercise improves lung function, while maintaining a healthy weight reduces strain on the respiratory system. Avoiding known triggers–such as pollen, pet dander, or smoke–is also crucial.
Alternative Therapies and Considerations
While some explore alternative therapies such as acupuncture or herbal remedies, scientific evidence supporting their effectiveness in managing asthma is limited. Always discuss any complementary treatments with your physician before starting them, especially if you’re already taking medication.
Treatment Selection: A Summary Table
| Treatment Type | Use Cases | Considerations |
|---|---|---|
| Inhaled Corticosteroids | First-line treatment for most asthma patients. | Most effective when used regularly. |
| Biologics | Severe asthma unresponsive to other therapies. | Requires specialist assessment and monitoring. |
| Leukotriene Modifiers | Add-on therapy for allergy-related or exercise-induced asthma. | May not be suitable for all patients. |
| Lifestyle Changes | Essential for all asthma patients to improve control. | Requires commitment and adherence to recommendations. |
Remember: This information is for educational purposes only and does not constitute medical advice. Always consult your doctor to develop a personalized asthma management plan.
When to Seek Immediate Medical Attention Regarding Prednisone and Asthma
Call emergency services immediately if you experience severe breathing difficulties, such as wheezing that doesn’t improve with your usual inhaler, or if you struggle to catch your breath.
Seek immediate medical attention if you develop chest pain, a rapid or irregular heartbeat, or feel dizzy or faint. These could indicate serious complications.
Contact your doctor or seek urgent care if you notice swelling of your face, lips, or tongue, or develop a rash. This might signal a severe allergic reaction.
High-dose prednisone can increase your risk of infection. If you develop a fever, chills, or worsening cough or other signs of infection, contact your doctor without delay.
Report any significant changes in your asthma symptoms, even if they seem unrelated to prednisone, to your healthcare provider. They can help you manage your condition safely and effectively.
Don’t hesitate to contact your doctor if you have any concerns about your prednisone treatment or your asthma control, no matter how minor they may seem.