Prednisone, a corticosteroid, can significantly reduce allergy symptoms, especially during severe flare-ups. It works by suppressing the body’s inflammatory response, thus alleviating swelling, itching, and breathing difficulties. However, it’s crucial to understand that Prednisone is not a long-term solution and carries potential side effects.
Your doctor might prescribe Prednisone for short-term relief from severe allergic reactions like acute asthma attacks or anaphylaxis. They’ll carefully determine the appropriate dosage and duration of treatment, tailored to your specific needs. Typical treatment courses range from a few days to a couple of weeks, depending on symptom severity.
Common side effects include increased appetite and weight gain, mood changes, insomnia, and increased blood sugar. Always inform your physician about any existing health conditions, current medications, and allergies before starting Prednisone. Regular monitoring of blood pressure and blood sugar might be necessary while on this medication. Remember to follow your doctor’s instructions precisely and report any concerning symptoms immediately. Long-term use increases the risk of more serious side effects, so adherence to the prescribed regimen is paramount.
Prednisone isn’t a substitute for long-term allergy management. It addresses acute symptoms but doesn’t address the underlying cause. Allergy testing and working with an allergist to develop a long-term management plan, including allergy shots or other medications, is recommended for lasting relief.
- Prednisone for Allergy Treatment: A Detailed Guide
- What is Prednisone and How Does it Work for Allergies?
- How Prednisone Affects Your Body
- Common Allergic Conditions Treated with Prednisone
- When is Prednisone Prescribed for Allergies?
- Severe Allergic Reactions Requiring Immediate Intervention
- Allergic Conditions Unresponsive to Standard Treatments
- Short-Term Use for Symptom Control
- Specific Conditions
- Dosage and Administration of Prednisone for Allergies
- Potential Side Effects of Prednisone for Allergy Relief
- Precautions and Contraindications of Prednisone Use
- Blood Pressure Monitoring
- Potential Side Effects and Precautions
- Prednisone vs. Other Allergy Medications: A Comparison
- Long-Term Use of Prednisone for Allergies: Risks and Benefits
- Potential Benefits of Long-Term Prednisone (Limited Circumstances)
- Risks of Long-Term Prednisone Use
- Alternatives to Long-Term Prednisone
- Managing Prednisone Use
- Disclaimer:
- Tapering Off Prednisone: A Safe and Effective Approach
- Recognizing and Managing Withdrawal Symptoms
- Monitoring Your Progress
Prednisone for Allergy Treatment: A Detailed Guide
Prednisone, a corticosteroid, powerfully reduces allergy symptoms by suppressing the immune system’s inflammatory response. Doctors prescribe it for severe allergic reactions unresponsive to other treatments.
Expect rapid symptom relief. However, Prednisone isn’t a long-term solution. Its use should be short-term, usually for a few days to a couple of weeks, to manage acute flare-ups.
Common side effects include increased appetite, weight gain, insomnia, and mood changes. Severe side effects are less common but require immediate medical attention. Always discuss potential side effects with your doctor before starting treatment.
Dosage varies based on your specific condition and response. Your physician will determine the optimal dose and duration. Never adjust your dosage independently; follow their instructions meticulously.
Prednisone can interact with other medications, including blood thinners and diabetes medication. Provide your doctor with a complete list of your current medications to prevent harmful interactions.
Gradually tapering off Prednisone is crucial to prevent withdrawal symptoms. Your doctor will guide you through a safe tapering schedule to minimize discomfort and ensure a smooth transition.
Prednisone should not be used during pregnancy or breastfeeding unless strictly necessary. Your physician will weigh the potential risks and benefits before making a recommendation.
Consult your doctor to confirm if Prednisone is appropriate for your allergy symptoms. They will evaluate your medical history and perform necessary tests before prescribing Prednisone or alternative treatments.
Always inform your doctor if you experience any unexpected symptoms while taking Prednisone. Prompt attention to potential problems ensures the safest possible treatment outcome.
What is Prednisone and How Does it Work for Allergies?
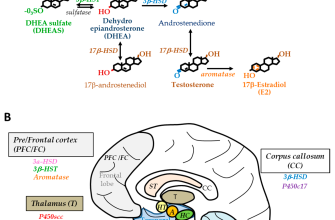
Prednisone is a corticosteroid medication, a powerful anti-inflammatory drug. It doesn’t directly block allergens; instead, it reduces your body’s allergic response. This means it lessens swelling, itching, and inflammation caused by allergens like pollen or pet dander.
How Prednisone Affects Your Body
Prednisone works by decreasing the production of substances your immune system releases during an allergic reaction. These substances, such as histamines and leukotrienes, are responsible for the uncomfortable symptoms you experience. By suppressing these, Prednisone provides significant relief.
Prednisone comes in different forms, including tablets. Your doctor determines the correct dosage and duration based on your specific allergy symptoms and health history. Always follow prescribed instructions. While effective for symptom management, Prednisone is not a long-term allergy solution and doesn’t prevent future allergic reactions. Your doctor may recommend other treatments alongside Prednisone for long-term allergy control, such as immunotherapy or allergy medication.
Common Allergic Conditions Treated with Prednisone
Prednisone, a corticosteroid, effectively manages inflammation associated with various allergies. It’s crucial to remember that it’s a powerful medication, and should only be used under a doctor’s supervision.
- Allergic Rhinitis (Hay Fever): Prednisone offers rapid relief from severe hay fever symptoms like sneezing, runny nose, and congestion, particularly during pollen season flare-ups. Short courses are usually prescribed.
- Asthma Exacerbations: In cases of severe asthma attacks, prednisone helps reduce airway inflammation and improve breathing. It’s often used alongside other asthma medications.
- Allergic Conjunctivitis: Prednisone eye drops may be prescribed for severe allergic eye inflammation. This manages itchiness, redness, and swelling.
- Severe Atopic Dermatitis (Eczema): For flare-ups of eczema causing significant skin irritation, prednisone can provide temporary relief. Topical steroids are usually preferred for long-term management.
- Angioedema: In cases of severe swelling, particularly affecting the face, lips, or throat, prednisone might be used to reduce inflammation and prevent airway obstruction. This is a medical emergency and requires immediate attention.
- Insect Sting Reactions: For severe allergic reactions to insect stings, prednisone may be part of the treatment plan to control inflammation and prevent complications. Epinephrine is the first-line treatment in these cases.
Note: This list isn’t exhaustive. Your doctor will determine the appropriate use of prednisone based on your specific allergy and its severity. They will also explain potential side effects and the duration of treatment.
- Always follow your doctor’s instructions precisely regarding dosage and duration.
- Never stop taking prednisone abruptly without consulting your physician. This should be done gradually to avoid withdrawal symptoms.
- Report any unusual side effects to your doctor immediately.
When is Prednisone Prescribed for Allergies?
Prednisone, a corticosteroid, treats severe allergic reactions that don’t respond to other medications. Doctors prescribe it for conditions like severe asthma exacerbations triggered by allergies, allergic reactions causing significant swelling (angioedema), or severe hives (urticaria) unresponsive to antihistamines.
Severe Allergic Reactions Requiring Immediate Intervention
Prednisone helps quickly reduce inflammation and control symptoms in life-threatening allergic reactions, such as anaphylaxis. It’s often part of a treatment plan alongside epinephrine and other supportive care.
Allergic Conditions Unresponsive to Standard Treatments
If your allergies are causing significant distress despite using antihistamines, decongestants, and other typical allergy medications, your doctor might consider prednisone. This is especially true for severe allergic rhinitis (hay fever) or allergic conjunctivitis.
Short-Term Use for Symptom Control
Prednisone’s role is typically short-term symptom management. It’s not a long-term solution for allergies; doctors generally prescribe it for a limited period to control a flare-up. Long-term use carries potential side effects, so careful monitoring is required.
Specific Conditions
Examples of allergic conditions potentially treated with prednisone include severe allergic reactions to insect stings or bites, acute exacerbations of allergic contact dermatitis, and certain types of vasculitis related to allergies.
Note: Always discuss allergy treatment options with your doctor. Prednisone has potential side effects, and the decision to use it depends on individual factors and the severity of your allergy symptoms.
Dosage and Administration of Prednisone for Allergies
Prednisone dosage for allergies depends entirely on the severity of your symptoms and your individual response. Your doctor will determine the appropriate dose.
Generally, treatment begins with a relatively high dose to quickly control symptoms. This dose is then gradually reduced over time as symptoms improve to minimize side effects.
- Typical starting doses for severe allergic reactions might range from 20-60 mg daily, taken once or in divided doses.
- Maintenance doses, once symptoms are controlled, are significantly lower, often between 5-10 mg daily, or even less.
- Treatment duration varies greatly and is determined by your doctor, based on your individual progress. It could range from a few days to several weeks. Long-term use requires close monitoring.
Prednisone is usually administered orally as a tablet. Always follow your doctor’s instructions regarding frequency of administration (once daily, twice daily, etc.).
- Take prednisone with food to reduce stomach upset.
- Never abruptly stop taking prednisone; gradually tapering the dose under your doctor’s guidance is crucial to prevent withdrawal symptoms.
- Be sure to inform your doctor about any other medications you are taking, as prednisone can interact with other drugs.
Remember: This information is for general knowledge only and should not substitute medical advice. Always consult with your doctor or other qualified healthcare professional to determine the best course of treatment for your specific situation and to discuss potential side effects. They will adjust your dosage and treatment plan according to your individual needs and response.
Potential Side Effects of Prednisone for Allergy Relief
Prednisone, while effective for allergy symptoms, can cause side effects. These vary depending on dosage and duration of treatment. Common side effects include increased appetite and weight gain. You may also experience fluid retention, leading to swelling in your ankles or face. Mood changes, such as irritability or anxiety, are also possible.
More serious, though less common, side effects can occur. These include increased blood sugar levels, potentially worsening existing diabetes. Prednisone can also weaken your immune system, making you more susceptible to infections. Increased blood pressure and thinning of bones (osteoporosis) are further possibilities.
Gastrointestinal problems, such as heartburn, nausea, or ulcers, are another concern. Skin changes like acne or thinning skin can also develop. Long-term use increases the risk of cataracts and glaucoma. Remember to discuss any concerns with your doctor.
It’s crucial to inform your doctor about all medications you take, including over-the-counter drugs and supplements, before starting prednisone. They can help manage potential side effects and ensure the safest treatment plan for your specific needs. Never stop taking prednisone suddenly; your doctor will guide you on a safe tapering schedule to minimize withdrawal symptoms.
Precautions and Contraindications of Prednisone Use
Always inform your doctor about all medications you take, including over-the-counter drugs and supplements, before starting prednisone. This helps prevent harmful interactions.
Prednisone can weaken your immune system, increasing your susceptibility to infections. Avoid contact with sick individuals and report any signs of infection immediately to your doctor.
Monitor your blood sugar regularly, especially if you have diabetes, as prednisone can raise blood glucose levels. Adjust your diabetes medication as needed under your doctor’s guidance.
Blood Pressure Monitoring
Prednisone may elevate your blood pressure. Regularly check your blood pressure and report any significant changes to your physician. They may adjust your medication accordingly.
Potential Side Effects and Precautions
| Side Effect | Precautions |
|---|---|
| Weight gain | Maintain a healthy diet and exercise regularly. Discuss weight management strategies with your doctor. |
| Mood changes | Be aware of changes in your mood and seek support if needed. Report any significant mood swings to your doctor. |
| Increased risk of osteoporosis | Maintain adequate calcium and vitamin D intake. Discuss bone health with your doctor, especially if you have risk factors for osteoporosis. |
| Gastrointestinal issues | Take prednisone with food to minimize stomach upset. Report any persistent gastrointestinal problems to your doctor. |
| Increased risk of cataracts and glaucoma | Undergo regular eye exams, especially if you have a history of eye problems. Report any vision changes promptly. |
Do not suddenly stop taking prednisone; gradually reduce the dosage under your doctor’s supervision to avoid withdrawal symptoms.
Prednisone is generally not recommended during pregnancy or breastfeeding unless the benefits clearly outweigh the potential risks. Discuss this with your doctor before becoming pregnant or during pregnancy or breastfeeding.
Individuals with certain medical conditions, such as active tuberculosis, peptic ulcers, or severe mental illness, should exercise extreme caution when considering prednisone. Your doctor can assess your suitability.
Prednisone vs. Other Allergy Medications: A Comparison
Prednisone, a corticosteroid, powerfully reduces allergy symptoms but isn’t a first-line treatment. It tackles inflammation swiftly, offering relief from severe reactions like anaphylaxis. However, its prolonged use carries risks, including weight gain and weakened immunity. Therefore, doctors typically prescribe it for short-term symptom control of severe allergies or when other medications fail.
Antihistamines, like cetirizine or fexofenadine, are usually the first choice for milder allergies. These work by blocking histamine, a chemical released during an allergic reaction, thus reducing symptoms such as itching, sneezing, and runny nose. They’re generally safe for long-term use, with fewer side effects than Prednisone.
Decongestants, such as pseudoephedrine or phenylephrine, relieve nasal congestion. These are often combined with antihistamines in over-the-counter medications. However, prolonged use can lead to rebound congestion, requiring careful monitoring.
Leukotriene modifiers, like montelukast, prevent inflammation. These are helpful for asthma and allergy symptoms, particularly nasal congestion and wheezing. They’re often used long-term and generally well-tolerated. However, their onset of action is slower than antihistamines or decongestants.
| Medication | Mechanism | Typical Use | Side Effects |
|---|---|---|---|
| Prednisone | Reduces inflammation | Severe allergies, short-term symptom control | Weight gain, weakened immunity |
| Antihistamines | Blocks histamine | Mild to moderate allergies | Drowsiness (some formulations) |
| Decongestants | Constricts blood vessels | Nasal congestion | Rebound congestion (with prolonged use), increased blood pressure |
| Leukotriene Modifiers | Inhibits inflammation | Asthma, allergic rhinitis | Headache, nausea (rare) |
Always consult your doctor to determine the best allergy treatment plan for your specific needs. They will consider your allergy severity, medical history, and potential drug interactions to select the safest and most effective medication.
Long-Term Use of Prednisone for Allergies: Risks and Benefits
Prednisone, while effective for allergy symptom relief, carries significant risks with prolonged use. Doctors generally avoid long-term prescriptions unless absolutely necessary because of potential side effects.
Potential Benefits of Long-Term Prednisone (Limited Circumstances)
- Severe, debilitating allergies unresponsive to other treatments: In rare cases, long-term prednisone might be the only option to manage life-threatening allergic reactions.
- Bridging therapy: It can be used temporarily while establishing alternative management strategies like immunotherapy.
Risks of Long-Term Prednisone Use
Extended prednisone use significantly increases the chance of adverse effects. These vary based on dosage and duration, but common risks include:
- Osteoporosis: Prednisone weakens bones, increasing fracture risk. Regular bone density monitoring is crucial.
- Weight gain: Fluid retention and altered metabolism often lead to significant weight increase.
- High blood pressure: Prednisone can elevate blood pressure, necessitating monitoring and potential medication adjustments.
- Increased blood sugar: Prednisone can raise blood glucose levels, posing a risk to diabetics and increasing the risk of developing diabetes.
- Cataracts and glaucoma: Long-term use can damage the eyes.
- Weakened immune system: Increased susceptibility to infections.
- Mood changes: Anxiety, depression, and irritability are common side effects.
- Thinning skin: Increased risk of bruising and slow wound healing.
- Muscle weakness: Prednisone can weaken muscles, impacting strength and physical function.
Alternatives to Long-Term Prednisone
Whenever possible, doctors favor safer, long-term allergy management strategies:
- Allergy shots (immunotherapy): Gradually desensitizes you to allergens, offering long-term relief.
- Other medications: Leukotriene inhibitors, mast cell stabilizers, and antihistamines provide longer-term relief with fewer risks than prednisone.
- Lifestyle changes: Identifying and avoiding allergens whenever possible.
Managing Prednisone Use
If long-term prednisone is unavoidable, close medical supervision is essential. Regular check-ups, blood tests, and monitoring of vital signs are crucial to detect and manage potential side effects. Gradual tapering of the dosage under a doctor’s guidance is also vital to minimize withdrawal symptoms and reduce the risk of relapse.
Disclaimer:
This information is for educational purposes only and should not be considered medical advice. Always consult your physician or allergist before starting or stopping any medication, especially long-term use of prednisone.
Tapering Off Prednisone: A Safe and Effective Approach
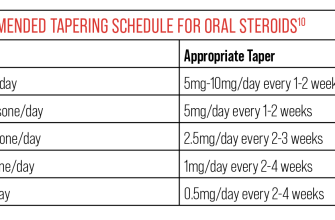
Always follow your doctor’s instructions for tapering. A common approach involves gradually reducing your dose by a small amount at regular intervals, typically every few days or weeks. For example, you might decrease your dose by 5mg every other day. This slow reduction allows your body to adjust naturally. Your doctor will personalize your tapering schedule based on your specific health condition, the duration of your prednisone use, and your individual response to the medication. Closely monitor yourself for any symptoms of withdrawal.
Recognizing and Managing Withdrawal Symptoms
Be aware that abruptly stopping prednisone can lead to serious withdrawal symptoms. Common symptoms include fatigue, muscle weakness, joint pain, nausea, and dizziness. Less common, but more severe, side effects are possible. Immediately contact your doctor if you experience any significant discomfort or worsening of existing conditions. Your doctor might need to adjust your tapering schedule to alleviate these symptoms. Stay hydrated and maintain a healthy diet to support your body during this transition.
Monitoring Your Progress
Regular check-ups with your doctor are critical. These appointments provide opportunities to assess your progress, monitor for any adverse effects, and make any necessary adjustments to the tapering plan. Open communication with your physician is crucial; don’t hesitate to report any concerns you may have. Maintaining a detailed record of your medication dosage and any symptoms you experience can be extremely helpful.