Prednisone can significantly reduce knee bursitis inflammation, offering quick pain relief. However, it’s crucial to understand its role as a short-term solution, not a long-term fix. We’ll explore its benefits, potential side effects, and how to best utilize it for optimal results.
Expect a reduction in swelling and pain within days of starting a Prednisone regimen, often prescribed as a short course (a few weeks). Your doctor will tailor dosage and duration to your specific needs, considering your medical history and the severity of your bursitis. Remember to closely follow their instructions.
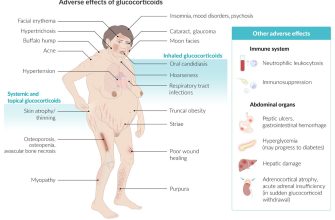
While Prednisone effectively manages inflammation, potential side effects like increased appetite, weight gain, insomnia, and mood changes might occur. Open communication with your physician about any symptoms is critical for managing these effects and ensuring safe usage. They can help you weigh the benefits against the potential drawbacks.
Beyond Prednisone, consider incorporating physical therapy, targeted exercises, and lifestyle adjustments to strengthen the knee and prevent future inflammation. These long-term strategies, combined with a properly managed course of Prednisone, offer a more holistic approach to managing knee bursitis.
Always consult your doctor before starting any medication, including Prednisone. They can provide personalized advice based on your individual health circumstances.
Prednisone for Knee Bursitis: When is it Necessary?
Prednisone, a powerful corticosteroid, isn’t always the first-line treatment for knee bursitis. Consider it when other methods fail. This typically means your pain is severe, significantly impacting your daily life, and unresponsive to conservative treatments like rest, ice, compression, and elevation (RICE) and over-the-counter pain relievers for at least several weeks.
Severe Pain and Functional Limitation
If your knee bursitis causes intense pain that prevents you from walking, climbing stairs, or performing everyday tasks, prednisone might be necessary to quickly reduce inflammation and provide pain relief. Consult your doctor if your pain persists despite several weeks of non-steroid treatments.
Failure of Other Treatments
Physicians typically prescribe physical therapy and other conservative methods before considering prednisone. If these approaches haven’t improved your condition within a reasonable timeframe (usually a few weeks), prednisone can offer a more rapid resolution to inflammation. Always discuss potential side effects with your doctor before starting prednisone.
Rapid Symptom Resolution
Prednisone’s strength lies in its ability to quickly reduce inflammation. If you need rapid relief – for instance, before a significant event – your doctor might recommend prednisone as a short-term solution to manage your symptoms. Remember, however, that prednisone is not a long-term solution and shouldn’t be used habitually.
Managing Prednisone Treatment for Knee Bursitis: Dosage, Side Effects, and Long-Term Considerations
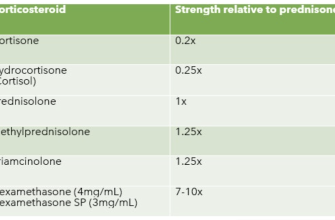
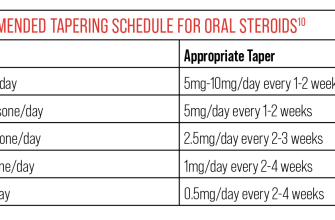
Your doctor will determine the appropriate prednisone dosage based on your specific needs and the severity of your bursitis. Typical dosages range from 5 to 60 milligrams daily, often starting high and tapering down gradually over several weeks. Never adjust your dosage without consulting your physician.
Common side effects include increased appetite, weight gain, mood swings, insomnia, and increased blood sugar. More serious, though less frequent, side effects may include increased risk of infection, osteoporosis, and cataracts. Report any unusual symptoms to your doctor immediately. Regular blood tests will monitor for potential complications.
Long-term prednisone use carries risks, so your doctor will strive for the shortest effective treatment duration. They might incorporate physical therapy, rest, and ice to reduce inflammation and promote healing. Discuss a plan to gradually reduce your prednisone dosage once your inflammation subsides to minimize withdrawal symptoms. This controlled reduction is key to prevent a relapse.
Remember, maintaining a healthy diet and regular exercise (as advised by your doctor) supports recovery and helps manage potential side effects. Open communication with your healthcare provider is vital for successful treatment and managing any complications that arise.