Prednisone isn’t a first-line treatment for low platelets (thrombocytopenia), but it can be helpful in specific situations. Doctors often consider it when the cause is an autoimmune disorder attacking your platelets, such as immune thrombocytopenic purpura (ITP).
Prednisone works by suppressing your immune system, reducing the destruction of platelets. Typical dosages range from 1 to 2 milligrams per kilogram of body weight daily. Your doctor will determine the appropriate dose and duration based on your individual needs and response to treatment. Expect regular blood tests to monitor your platelet count and assess the Prednisone’s effectiveness.
Important Note: Prednisone carries potential side effects, including weight gain, increased blood sugar, and increased risk of infection. Open communication with your doctor is critical; report any concerning symptoms promptly. They’ll balance the benefits of increased platelet count against potential side effects, adjusting treatment accordingly.
Remember: This information is for educational purposes only and does not constitute medical advice. Always consult with your physician or a qualified healthcare professional before starting any new medication, including Prednisone, to discuss whether it’s the right treatment option for your specific condition and to manage potential risks.
- Prednisone for Low Platelets: A Detailed Guide
- Identifying the Root Cause
- Prednisone’s Role and Limitations
- Alternative and Complementary Treatments
- Understanding Thrombocytopenia and its Causes
- Common Causes of Low Platelets
- Less Common Causes
- Prednisone’s Role in Treating Low Platelets
- How Prednisone Affects Platelet Levels
- Important Considerations When Using Prednisone
- Prednisone and Other Treatments
- Monitoring Your Progress
- Dosage, Administration, and Potential Side Effects
- Alternative Treatments and Long-Term Management
- Lifestyle Adjustments
- Medical Interventions
- Long-Term Monitoring and Management
- Addressing Underlying Conditions
Prednisone for Low Platelets: A Detailed Guide
Prednisone, a corticosteroid, can sometimes help raise low platelet counts (thrombocytopenia). It works by suppressing the immune system, which may be attacking platelets in certain autoimmune conditions. However, it’s not a first-line treatment and its use depends heavily on the underlying cause of the low platelets.
Identifying the Root Cause
Before considering Prednisone, your doctor must determine *why* your platelet count is low. Common causes include autoimmune diseases (like ITP), infections, medications, and certain cancers. Diagnostic tests like a complete blood count (CBC), peripheral blood smear, and bone marrow biopsy may be necessary to pinpoint the problem. Treatment focuses on addressing this underlying issue.
Prednisone’s Role and Limitations
If your low platelets are due to an autoimmune disorder, Prednisone might be prescribed to reduce immune system activity and allow your body to produce more platelets. Typical dosages and treatment durations vary significantly depending on your individual condition and response to treatment. Expect close monitoring of your platelet count and overall health during treatment. Prednisone is not a cure; it manages symptoms. Side effects, which can be significant, should be discussed with your physician. These can include weight gain, increased blood sugar, and increased risk of infection. Furthermore, Prednisone may not be effective for all forms of thrombocytopenia.
Alternative and Complementary Treatments
Other treatment options for low platelets exist, including intravenous immunoglobulins (IVIG), rituximab, and splenectomy (removal of the spleen). Your doctor will consider these and other therapies, tailoring a treatment plan to your specific situation. Always follow your doctor’s recommendations closely and report any unusual symptoms or concerns.
Understanding Thrombocytopenia and its Causes
Thrombocytopenia signifies a low platelet count, impacting your blood’s ability to clot. A normal platelet count generally ranges from 150,000 to 450,000 per microliter of blood. Counts below 150,000 indicate thrombocytopenia, and lower counts increase bleeding risk.
Common Causes of Low Platelets
Many factors contribute to low platelet counts. Decreased platelet production in the bone marrow is a frequent culprit. This can stem from various conditions like aplastic anemia (bone marrow failure), leukemia (cancer of the blood cells), and certain viral infections, such as HIV or hepatitis. Autoimmune diseases, where the body attacks its own cells, often target platelets, leading to their destruction. Examples include immune thrombocytopenic purpura (ITP) and systemic lupus erythematosus (SLE).
Increased platelet destruction is another significant cause. Besides autoimmune disorders, this can be triggered by medications, such as heparin (a blood thinner), or certain infections. Sometimes, platelets are destroyed within the spleen, an organ that filters blood. This can occur in splenomegaly (enlarged spleen).
Less Common Causes
Inherited disorders affecting platelet function or production are less frequent causes of thrombocytopenia. These are usually diagnosed in childhood or early adulthood. Platelet sequestration, where platelets accumulate in the spleen, can also contribute to low counts. Finally, various conditions affecting bone marrow function, such as chemotherapy or radiation therapy, can temporarily lower platelet production.
Prednisone’s Role in Treating Low Platelets
Prednisone, a corticosteroid, sometimes helps raise low platelet counts (thrombocytopenia). It works by suppressing the immune system, which can be attacking platelets in conditions like immune thrombocytopenic purpura (ITP).
How Prednisone Affects Platelet Levels
Prednisone reduces the destruction of platelets by immune cells. This leads to a higher platelet count. The dosage and duration of treatment vary widely based on the severity of thrombocytopenia and individual patient response. Your doctor will determine the appropriate course of action.
Important Considerations When Using Prednisone
Prednisone’s effects aren’t immediate. Improvement in platelet count usually takes several days to weeks. Regular blood tests monitor your platelet levels and the prednisone’s efficacy. Long-term prednisone use carries side effects like weight gain, increased blood sugar, and weakened bones. Your doctor will carefully weigh the benefits against these risks.
Prednisone and Other Treatments
Prednisone is often used as a first-line treatment for ITP, but it might be combined with other medications or treatments, such as intravenous immunoglobulins (IVIG) or splenectomy, depending on your condition’s response.
| Treatment Approach | Description |
|---|---|
| Prednisone Monotherapy | Prednisone is the sole treatment. |
| Prednisone and IVIG | Prednisone is used in conjunction with intravenous immunoglobulins. |
| Prednisone and Splenectomy | Prednisone is used alongside surgical removal of the spleen. |
Monitoring Your Progress
Frequent blood tests are critical to track your platelet count and ensure the treatment’s effectiveness. Close communication with your healthcare provider is vital throughout the treatment process to adjust the medication as needed and address any side effects promptly.
Dosage, Administration, and Potential Side Effects
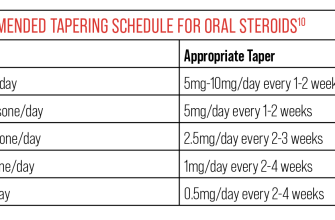
Prednisone dosage for low platelets (thrombocytopenia) varies greatly depending on the severity of the condition and the individual’s response. Your doctor will determine the appropriate dose, typically starting with a higher dose and gradually tapering it down as your platelet count improves. This is usually administered orally, once or twice daily, with food to minimize stomach upset.
Common side effects include increased appetite and weight gain, fluid retention (swelling), mood changes, insomnia, and increased blood sugar. More serious, though less common, side effects involve increased risk of infection, weakened bones (osteoporosis), high blood pressure, and cataracts. If you experience severe side effects or your platelet count doesn’t improve, contact your doctor immediately.
Regular monitoring of your platelet count and overall health is critical while taking prednisone. Your physician will schedule blood tests to assess your progress and adjust your medication as needed. Open communication with your doctor about any concerns or side effects is highly recommended. Remember, adhering to the prescribed dosage and schedule is crucial for effective treatment.
Alternative Treatments and Long-Term Management
Addressing low platelet counts (thrombocytopenia) often requires a multifaceted approach beyond prednisone. Your doctor will tailor treatment to the underlying cause.
Lifestyle Adjustments
- Dietary modifications: A diet rich in vitamin K, folate, and B12 can support platelet production. Consult a nutritionist for personalized recommendations.
- Alcohol reduction or cessation: Alcohol can impair platelet function and production. Limiting or eliminating alcohol consumption is crucial.
- Regular exercise: Moderate physical activity promotes overall health, potentially aiding in blood cell production.
Medical Interventions
Depending on the cause and severity, alternative treatments might include:
- Immunosuppressants: These medications suppress the immune system’s attack on platelets. Examples include azathioprine or cyclosporine.
- Intravenous immunoglobulin (IVIG): This treatment helps improve platelet counts by modulating the immune response.
- Platelet transfusions: In cases of severe thrombocytopenia, transfusions provide immediate platelet replenishment.
- Romiplostim or eltrombopag: These medications stimulate platelet production in the bone marrow.
- Splenectomy: In certain autoimmune conditions, surgical removal of the spleen may be considered, as the spleen often destroys platelets.
Long-Term Monitoring and Management
- Regular blood tests: Consistent monitoring of platelet counts is essential to track response to treatment and identify potential problems.
- Close physician follow-up: Maintaining regular communication with your hematologist is crucial for ongoing management and adjustments to therapy.
- Understanding potential complications: Be aware of the signs and symptoms of bleeding and seek immediate medical attention if they arise.
- Medication adherence: Strictly follow your prescribed medication regimen as instructed by your doctor.
Addressing Underlying Conditions
Successfully managing low platelets necessitates addressing the underlying cause. This might involve treating an infection, managing an autoimmune disorder, or addressing other medical conditions.