Reduce your prednisone dose gradually, ideally under a doctor’s supervision, following a personalized schedule. This slow reduction minimizes the risk of withdrawal symptoms, including depression.
Monitor your mood closely during the tapering process. Report any significant changes, like increased sadness, irritability, or loss of interest in activities, to your physician immediately. Early intervention is key.
Consider adding a support system. Talk to family, friends, or a therapist about your experience. Sharing your feelings can significantly reduce stress and improve coping mechanisms during this challenging transition.
Explore complementary therapies alongside medical care. Activities like gentle exercise, mindfulness techniques, and sufficient sleep can naturally boost mood and improve overall well-being while tapering. Discuss these options with your doctor.
Remember, a healthy diet and regular physical activity play a significant role in stabilizing mood. Focus on nutritious food choices and incorporate regular movement into your daily routine to support your mental and physical health.
Always consult your doctor before making any changes to your medication regimen or incorporating new therapies. They can tailor a plan specific to your needs and medical history, ensuring a safe and effective tapering process.
- Tapering Off Prednisone and Depression: A Practical Guide
- Managing Withdrawal Symptoms
- Lifestyle Adjustments
- Medication and Therapy
- Monitoring Your Progress
- Understanding Prednisone’s Impact on Mood
- Recognizing Depression Symptoms During Tapering
- Changes in Appetite and Energy
- Cognitive Changes to Watch For
- When to Seek Help
- The Importance of a Gradual Tapering Schedule
- Understanding the Risks of Sudden Withdrawal
- Following Your Doctor’s Plan
- Common Tapering Schedules
- Monitoring Your Progress
- Managing Depression During Tapering
- Remember
- Communicating with Your Doctor: Essential Steps
- Lifestyle Adjustments for Mood Support
- Nutrition for a Better Mood
- Coping Mechanisms for Depression During Withdrawal
- Dietary Changes
- Connecting with Others
- Seeking Professional Support
- Mindfulness Techniques
- Seeking Additional Support: Therapy and Medication
- Long-Term Mental Health Strategies After Prednisone
- Lifestyle Changes for Sustained Well-being
Tapering Off Prednisone and Depression: A Practical Guide
Consult your doctor before making any changes to your prednisone dosage. They can create a personalized tapering schedule based on your specific needs and medical history. A slow, gradual reduction is key to minimizing withdrawal symptoms.
Managing Withdrawal Symptoms
Expect potential side effects like fatigue, joint pain, and mood changes (including depression). Keep a detailed symptom diary, noting severity and timing. This information helps you and your doctor track progress and adjust the tapering schedule as needed. Consider discussing additional support, like therapy or medication for depression, with your doctor *before* starting the taper. This proactive approach can help manage mood swings.
Lifestyle Adjustments
Prioritize adequate sleep, aiming for 7-9 hours per night. Regular exercise, even short walks, improves mood and energy levels. A balanced diet rich in fruits, vegetables, and whole grains provides essential nutrients. Minimize stress through relaxation techniques like yoga or deep breathing. Maintain open communication with your doctor and support network. Share any concerns or changes in your condition immediately.
Medication and Therapy
Your doctor might prescribe antidepressants or other medications to help manage depression during and after the prednisone taper. Consider cognitive behavioral therapy (CBT) or other therapeutic interventions. These can provide coping strategies and help address underlying emotional issues, further aiding your recovery. Regular check-ups with both your physician and therapist ensure ongoing monitoring and support.
Monitoring Your Progress
Track your mood daily, using a scale (e.g., 1-10). Note any changes in sleep, appetite, or energy levels. Regular blood tests may be needed to monitor your cortisol levels and overall health. Openly discuss all aspects of your experience with your healthcare team – honesty is crucial for effective treatment.
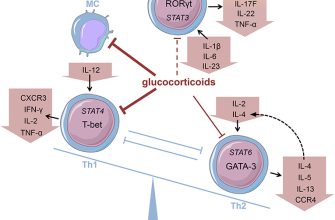
Understanding Prednisone’s Impact on Mood
Prednisone, a powerful corticosteroid, can significantly affect your mood. Many experience mood swings, ranging from mild irritability to severe depression.
Here’s what you should know:
- Increased risk of depression: Studies show a correlation between prednisone use and an increased risk of developing depression, especially with higher doses and longer treatment durations.
- Mechanism: Prednisone alters neurotransmitter levels in the brain, impacting mood regulation. This disruption can manifest as anxiety, irritability, euphoria, or depression.
- Symptoms: Watch for persistent sadness, loss of interest in activities, changes in sleep patterns (insomnia or hypersomnia), fatigue, feelings of worthlessness, and difficulty concentrating.
Managing mood changes during prednisone treatment is crucial. Here are some strategies:
- Open communication with your doctor: Report any mood changes immediately. They can adjust your dosage or prescribe additional medication to help.
- Lifestyle adjustments: Prioritize sleep, eat a balanced diet, and engage in regular physical activity. These lifestyle choices can significantly improve mood.
- Consider therapy: Cognitive Behavioral Therapy (CBT) can provide coping mechanisms for managing mood fluctuations.
- Support system: Lean on family and friends for emotional support during this time. Their understanding can make a real difference.
Remember, tapering off prednisone requires careful monitoring. Your doctor will guide you through this process, helping to minimize potential mood disturbances. Always adhere to your prescribed tapering schedule.
It’s important to remember that individual responses to prednisone vary. What works for one person may not work for another. Close collaboration with your healthcare provider is key to successfully managing both your physical and mental health during and after prednisone treatment.
Recognizing Depression Symptoms During Tapering
Monitor your mood closely. Increased sadness, irritability, or anxiety are common. Pay attention to changes in your sleep patterns – insomnia or excessive sleeping are significant indicators.
Changes in Appetite and Energy
Track your appetite. Notice significant weight loss or gain. Fatigue and lack of energy are frequent symptoms; a decreased interest in activities you once enjoyed is another red flag.
Cognitive Changes to Watch For
Difficulty concentrating and making decisions is a major warning sign. Feelings of hopelessness and worthlessness are serious and require immediate attention. Consider keeping a mood journal to track these changes.
When to Seek Help
Contact your doctor immediately if you experience suicidal thoughts or intense feelings of despair. Don’t hesitate to reach out to a mental health professional for support during this challenging time. They can provide guidance and potentially adjust your treatment plan.
The Importance of a Gradual Tapering Schedule
Your doctor will create a personalized prednisone tapering schedule. This schedule is vital for minimizing withdrawal symptoms, including depression. Rapid reduction can trigger severe side effects.
Understanding the Risks of Sudden Withdrawal
Stopping prednisone abruptly can lead to:
- Extreme fatigue
- Muscle weakness
- Joint pain
- Nausea and vomiting
- Severe depression
- Adrenal insufficiency
These symptoms can significantly impact your daily life and mental well-being.
Following Your Doctor’s Plan
Adherence to your prescribed tapering schedule is paramount. Typical schedules involve gradually decreasing your dose over several weeks or months. This slow reduction allows your body to adjust naturally.
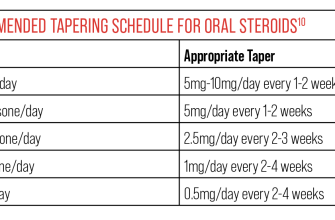
Common Tapering Schedules
While individual schedules vary, common approaches include:
- Reducing the daily dose by a small percentage (e.g., 5-10%) every few days or weeks.
- Alternating days of lower doses.
- Switching to every-other-day dosing before fully stopping.
Monitoring Your Progress
Regular check-ups with your doctor are necessary. They will monitor your progress, adjust the schedule if needed, and address any arising concerns. Open communication about your physical and emotional state is key.
Managing Depression During Tapering
Many experience mood changes during prednisone withdrawal. Your doctor might recommend strategies such as therapy, antidepressants, or other supportive measures to manage these symptoms.
Remember
Patient cooperation and close medical supervision are crucial for a safe and successful prednisone taper.
Communicating with Your Doctor: Essential Steps
Keep a detailed journal tracking your mood, prednisone dosage, and any physical symptoms. This provides valuable data for your doctor.
Schedule regular appointments to discuss your progress and any concerns. Frequency depends on your individual needs but aim for consistent monitoring during tapering.
Clearly articulate your symptoms, using specific examples. Instead of “I feel bad,” describe your feelings: “I experience persistent fatigue and low mood, impacting my daily activities.”
Be honest about your adherence to the medication schedule. Report any missed doses or difficulties with the tapering plan.
Actively participate in the discussion. Ask clarifying questions about the tapering process and potential side effects. Don’t hesitate to voice concerns.
Discuss potential alternative treatments for depression if needed. Collaborate with your doctor to find the best approach for your situation.
Bring a friend or family member to appointments for support and to help remember information discussed.
Follow your doctor’s instructions carefully and maintain open communication throughout the process. This collaborative approach ensures the best outcome.
Lifestyle Adjustments for Mood Support
Prioritize sleep: Aim for 7-9 hours of quality sleep nightly. Establish a consistent sleep schedule, even on weekends, to regulate your body’s natural sleep-wake cycle. Create a relaxing bedtime routine to wind down before sleep, avoiding screen time at least an hour before bed.
Nutrition for a Better Mood
Nourish your body with nutrient-rich foods. Focus on whole, unprocessed foods like fruits, vegetables, lean proteins, and whole grains. Limit processed foods, sugary drinks, and excessive caffeine, which can negatively impact mood and energy levels. Consider adding foods rich in omega-3 fatty acids, like salmon or flaxseed, known for their mood-boosting properties.
Increase physical activity: Regular exercise releases endorphins, natural mood boosters. Aim for at least 30 minutes of moderate-intensity exercise most days of the week. Find activities you enjoy, whether it’s walking, swimming, cycling, or yoga, to ensure consistency. Even short bursts of activity throughout the day can make a difference.
Practice mindfulness and stress reduction techniques: Incorporate mindfulness exercises like meditation or deep breathing into your daily routine. These techniques can help manage stress and anxiety, common side effects of prednisone withdrawal. Consider yoga or Tai Chi for both physical and mental benefits.
Connect with others: Maintain strong social connections. Spend time with loved ones, participate in social activities, or join a support group. Social interaction provides emotional support and reduces feelings of isolation, which is particularly important during periods of mood change.
Sunlight exposure: Get at least 15 minutes of sunlight daily. Sunlight helps regulate your circadian rhythm and boosts vitamin D levels, which are linked to mood. A simple walk outside can be beneficial.
Coping Mechanisms for Depression During Withdrawal
Prioritize regular, moderate exercise. Aim for at least 30 minutes most days. Walking, swimming, or cycling are excellent choices. Physical activity releases endorphins, naturally improving mood.
Engage in activities you enjoy. This could be anything from reading to gardening to listening to music. Schedule these activities into your day, making them a non-negotiable part of your routine. Even small pleasures accumulate.
Maintain a consistent sleep schedule. Try to go to bed and wake up around the same time each day, even on weekends. Aim for 7-9 hours of sleep. A regular sleep pattern regulates your body’s natural rhythms, positively affecting mood.
Dietary Changes
Focus on a balanced diet rich in fruits, vegetables, and whole grains. Limit processed foods, sugar, and caffeine. These dietary adjustments can significantly impact energy levels and mood.
Connecting with Others
Spend time with loved ones. Social interaction is crucial for mental well-being. Reach out to friends and family, or consider joining a support group. Talking about your feelings can be incredibly helpful.
| Day | Activity | Mood Rating (1-10) |
|---|---|---|
| Monday | 30-minute walk, light reading | |
| Tuesday | Yoga class, dinner with friend | |
| Wednesday | Gardening, listening to music |
Track your mood daily. Use a journal or app to monitor your feelings. Identifying patterns can help you understand triggers and adjust coping strategies accordingly.
Seeking Professional Support
Don’t hesitate to contact your doctor or therapist. They can provide additional support and guidance during this challenging time. Medication adjustments or therapy may be beneficial.
Mindfulness Techniques
Practice mindfulness techniques like meditation or deep breathing exercises. These can help you manage stress and anxiety, common side effects of prednisone withdrawal.
Seeking Additional Support: Therapy and Medication
Consider cognitive behavioral therapy (CBT) to manage depression symptoms related to prednisone withdrawal. CBT teaches coping mechanisms for negative thoughts and behaviors. Find a therapist specializing in mood disorders and medication management.
Your doctor might prescribe antidepressants, such as SSRIs or SNRIs, to alleviate depression during and after tapering. Discuss potential side effects and medication interactions with your physician. Maintain open communication about your symptoms’ response to treatment.
Support groups offer a safe space to share experiences and connect with others facing similar challenges. Online forums and local meetings can provide valuable emotional support and practical advice. Explore resources like the Depression and Bipolar Support Alliance (DBSA).
Regular exercise, a balanced diet, and sufficient sleep significantly impact mood. Aim for at least 30 minutes of moderate-intensity exercise most days of the week. Prioritize nutritious foods and consistent sleep schedules.
Note: This information is for general knowledge and does not constitute medical advice. Always consult your doctor or other qualified healthcare professional for diagnosis and treatment of any medical condition.
Long-Term Mental Health Strategies After Prednisone
Maintain open communication with your doctor and psychiatrist throughout the tapering process and beyond. Regular check-ups allow for adjustments to medication and prompt addressing of any emerging concerns.
Consider incorporating mindfulness techniques like meditation or deep breathing exercises into your daily routine. Aim for at least 10 minutes daily to reduce stress and improve mood regulation. Apps like Calm or Headspace can guide you.
Lifestyle Changes for Sustained Well-being
Prioritize regular physical activity. Aim for at least 150 minutes of moderate-intensity aerobic exercise per week. Even short walks can significantly boost mood and reduce anxiety.
Ensure adequate sleep. Aim for 7-9 hours of quality sleep each night. Establish a consistent sleep schedule and create a relaxing bedtime routine. Consult a sleep specialist if you face difficulties.
Nourish your body with a balanced diet rich in fruits, vegetables, and whole grains. Limit processed foods, sugar, and caffeine, as these can negatively impact mood.
Build a strong support system. Connect with friends, family, or support groups. Sharing your experiences can alleviate feelings of isolation and provide emotional support.
Explore therapeutic options. Cognitive Behavioral Therapy (CBT) and other therapies can equip you with coping mechanisms for managing stress and improving mental health. Don’t hesitate to seek professional help if you need it.